Hidden Penis Surgery: Solutions for Hygiene, Infection, and Sexual Health
9/3/2025
Explore surgery to correct for hidden penis, addressing issues like hygiene, infection, and sexual health—expert solutions for confidence and well-being.
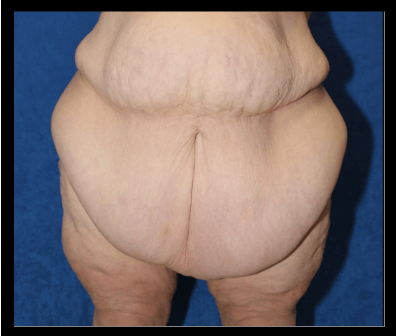
Figure 1. Picture of a hidden penis due to obesity and weight loss.
Introduction to Hidden Penis: Understanding the Condition
Hidden penis, also referred to as "buried penis," is a medical condition characterized by the incomplete visibility of the penis. In this condition, the penis may appear to be retracted or concealed under the surrounding skin, fat, or connective tissues. While this condition can affect both children and adults, its causes, symptoms, and treatment options vary depending on the patient's age and overall health. Understanding the underlying factors contributing to this issue is crucial in addressing its physical and psychological impacts.
The primary causes of a hidden penis can include excess adipose tissue around the pubic area, congenital abnormalities, post-surgical complications, or scarring due to trauma or infection. In some cases, obesity plays a significant role as an accumulation of fat may obscure otherwise normal penile anatomy. Other contributing factors include poorly attached skin, weak suspensory ligaments, or conditions such as lymphedema, which can lead to swelling and concealment.
This condition is not merely a cosmetic concern—it often presents challenges in daily life. Hygiene can become a significant problem, as the concealed penis may trap moisture and bacteria, leading to discomfort and an increased risk of infections. Additionally, sufferers often experience irritation, difficulty with urination, and complications during intimate relationships. Over time, these issues may adversely affect self-esteem and mental health.
Plastic surgeons emphasize the importance of diagnosing a hidden penis through physical examination and medical history assessment. Such evaluations help determine the severity of the condition and guide the selection of appropriate treatment options, which may range from non-surgical interventions to corrective surgery. Understanding the intricacies of the hidden penis provides the groundwork for addressing its functional and psychological repercussions effectively.
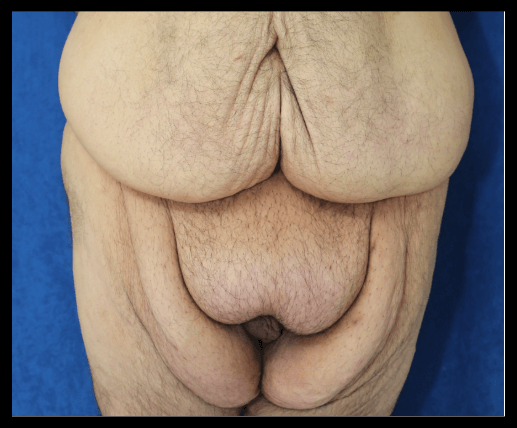
Figure 2: Hidden penis due to history of obesity and significant weight loss
Causes of Hidden Penis: Beyond Confusion and Misconception
A hidden or buried penis is a medical condition often surrounded by confusion and misconceptions, yet its causes are rooted in identifiable physical and developmental factors. It involves the concealment of the penile shaft beneath excess skin, fat, or other anatomical structures, which can lead to hygiene complications, infections, and issues with sexual function. Understanding the underlying causes is crucial to effectively addressing this condition.
-
Congenital Factors
-
Some cases of hidden penis are congenital, originating from improper development in utero. This can result from a deficiency in connective tissue or structural abnormalities of the skin and surrounding area during fetal growth.
-
Weak suspensory ligaments in the penile region may prevent adequate anchorage of the organ, causing it to become recessed or hidden within the pubic tissue.
-
-
Obesity
-
Excessive subcutaneous fat in the pubic region is a leading contributor to acquired hidden penis. In obese individuals, fat buildup around the lower abdomen may envelop the penile shaft, making it less visible.
-
Obesity increases the risk of difficulty maintaining hygiene, which can exacerbate secondary complications like infections and skin irritation.
-
-
Scar Tissue and Trauma
-
Post-surgical complications, injuries, or surgical procedures in the genital or abdominal areas may lead to scarring. Excess scar tissue can pull the penis inward or obstruct its appearance.
-
Retractile effects from scar formation around the lower abdomen or penile base make certain medical conditions prone to the development of a hidden penis.
-
-
Penile Skin Laxity
-
Excessive or loose penile skin can result in the structure being partially enveloped. This penis skin laxity often occurs in older adults due to loss of elasticity, though it may also develop in younger individuals with certain dermatological conditions.
-
- Lymphedema and Medical Conditions
-
Conditions affecting lymphatic drainage in the groin area, such as lymphedema, can cause swelling that obstructs or conceals the penis.
-
Other health issues, including hormonal imbalances or diabetes-related complications, may indirectly contribute by worsening structural or skin-related factors.
-
Understanding hidden penis requires a shift in focus from misconceptions to objective causes such as anatomy, weight, and surgical outcomes. This knowledge paves the way for effective corrective measures.
The Impact of Hidden Penis on Hygiene and Daily Life
A hidden penis, medically known as a concealed or buried penis, can significantly influence hygiene and daily living. This condition, characterized by the penile shaft being obscured by surrounding tissue or skin, often presents challenges in maintaining proper hygiene and managing general self-care routines. The consequences of this can affect physical health and emotional well-being.
Hygiene Challenges
Individuals with a hidden penis frequently experience difficulty in accessing and cleaning the genital area. This limited access can cause a buildup of sweat, urine, and dead skin cells, leading to unpleasant odors and an increased risk of bacterial or fungal infections. Persistent moisture and inadequate ventilation around the genital region can further exacerbate these issues, making it challenging to maintain optimal hygiene.
If cleaning becomes cumbersome, the affected individual may develop conditions such as balanitis, characterized by inflammation of the glans penis. Moreover, the accumulation of debris can cause discomfort or irritation, discouraging proper hygiene practices altogether.
Effects on Daily Life
The impact of a hidden penis extends beyond physical health, influencing psychological and practical aspects of daily routines. Many individuals report feelings of embarrassment, diminished confidence, or social discomfort due to the condition, which can erode self-esteem over time. Difficulty performing normal personal hygiene tasks may also contribute to an ongoing sense of frustration, potentially interfering with one's ability to focus on daily responsibilities or interact socially.
Certain activities, like exercising, may become more uncomfortable due to chafing or friction. Clothing choices may need to be adjusted to accommodate discomfort or concerns about concealment. These adaptations can disrupt typical routines and contribute to emotional strain.
Addressing the impact holistically often requires professional intervention, focusing on hygiene education, personalized strategies, and medical solutions to improve health and daily functioning.
Infection Risks Associated with Hidden Penis
A hidden penis condition can pose significant risks related to infections due to limited external exposure and compromised hygiene. When the penis remains buried beneath surrounding tissues, it creates a warm and moist environment that may foster bacterial and fungal growth. This environment significantly increases the predisposition to local and systemic infections, necessitating prompt and effective management strategies.
The accumulation of sweat, dead skin cells, and urine residue in the folds surrounding the hidden penis can lead to localized conditions such as intertrigo and balanitis. Intertrigo, characterized by chafed, inflamed skin within folds, often results from friction and microbial growth. Balanitis, a common infection affecting the foreskin and glans, typically arises due to poor aeration and inadequate hygiene practices in uncircumcised penis cases. Both conditions may cause redness, swelling, discharge, and discomfort, requiring medical attention.
Further complications are associated with recurrent infections that may progress to cellulitis or abscess formation. Cellulitis is a deep skin infection that can spread rapidly, leading to systemic issues such as fever and chills if left untreated. In severe cases, chronic irritation and untreated infections may increase the risk of fibrosis in surrounding tissues, complicating surgical interventions.
Patients with diabetes or obesity face additional risk, as these conditions exacerbate immune system challenges and enhance microbial propagation. Impaired glucose regulation in people with diabetes further heightens the likelihood of fungal infections such as candidiasis in the genital folds.
Preventative measures require diligent personal hygiene, including routine washing with non-irritating cleansers to prevent debris buildup. A medical evaluation may be necessary to address recurring infections or associated complications, such as lymphedema. Surgical correction can reduce infection risks by effectively addressing the underlying structural issues associated with the condition.
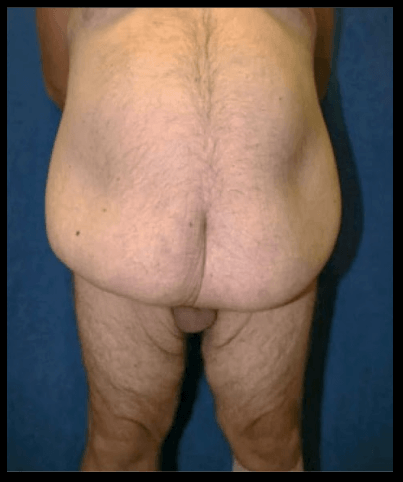
Figure 3: Picture of hidden penis due to excess skin and fat in supra-pubic region and lower abdomen.
Psychological and Emotional Challenges of Hidden Penis
The condition known as hidden penis can pose significant psychological and emotional challenges for affected individuals, impacting their quality of life, confidence, and mental well-being. These challenges often stem from the interplay of physical concerns, societal attitudes, and deeply personal body image struggles.
-
Emotional Distress and Body Image Concerns
A hidden penis is often accompanied by a profound sense of embarrassment or shame, as individuals may feel their bodies are out of alignment with societal expectations of male anatomy. Negative self-perception may lead to recurring feelings of worthlessness, inadequacy, or frustration. Many individuals with a hidden penis face difficulties in accepting their appearance, which can lead to chronic body dissatisfaction and emotional turmoil.
-
Social Anxiety and Fear of Judgment
The fear of being judged or misunderstood causes many affected individuals to avoid social situations where their condition might be disclosed, either inadvertently or through routines such as intimate relationships, public restrooms, or medical examinations. This avoidance can foster feelings of isolation, contributing to long-term anxiety and worsening emotional distress. For some, the condition becomes a source of heightened social anxiety that interferes with personal and professional life.
-
Impacts on Sexual Identity and Relationships
A hidden penis may profoundly affect an individual's sexual identity and intimacy. Challenges with sexual function or appearance can generate self-doubt, fear of rejection, or a decreased willingness to engage in physical relationships. These issues, in turn, may lead to strained relationships or difficulties forming intimate connections. The embarrassment and psychological barriers tied to the condition often exacerbate emotional struggles in romantic contexts.
-
Risk of Depression and Other Mental Health Disorders
When left unaddressed, the persistent feelings of hopelessness and internalized shame associated with a hidden penis may escalate into more serious mental health conditions, such as depression or heightened stress. This makes timely intervention—surgical, therapeutic, or both—essential, allowing individuals to regain confidence and improve their emotional well-being over time.
Hidden penis surgery and associated treatments aim to minimize these psychological and emotional challenges by addressing the physical aspect of the condition while supporting individuals in reclaiming a sense of normalcy and emotional stability.
Medical and Surgical Solutions: Overview of Treatment Options
A hidden penis, also known as a buried or concealed penis, can pose challenges related to hygiene, infection, and sexual health. Treatment options vary depending on the underlying causes and the patient's health. Professionals approach this condition with various medical and surgical interventions tailored to meet individual needs, ensuring both physical and psychological concerns are addressed.
-
Medical Treatment Options
Non-surgical interventions are often the first course of action for mild cases or when surgery is contraindicated. These options may include:
-
Weight Loss and Nutritional Intervention
Excess fat in the pubic region is a common contributing factor to this condition. Weight reduction strategies, guided by registered dietitians, can help restore the natural appearance.
-
Topical or Oral Medications
In cases involving skin irritation or fungal infections, plastic surgeons may prescribe antifungal creams, antibiotics, or anti-inflammatory medications to manage symptoms.
-
Stretching and Skin Therapy
Dermatological treatments, such as stretching the affected area, may be recommended to improve skin elasticity and reduce complications associated with phimosis. Stretching treatments can include pressured suction devices.
-
Surgical Treatment Options: Plastic surgery is often considered when medical approaches fail to achieve desired outcomes. Surgical options include:
-
Penile Release Surgery: A procedure that frees the concealed penis from surrounding tissue and structures is commonly employed. This repositions the penis for optimal function and visibility.
-
Urethral Reconstruction: For cases involving urinary complications, procedures may correct any anatomical abnormalities affecting urination.
-
Fat Pad Removal (Lipectomy): Excess fatty tissue in the suprapubic area can be excised to eliminate barriers concealing the penis.
-
Circumcision: In some cases, circumcision is performed to address issues related to tight foreskin or chronic infections, aiding in hygiene maintenance and reducing recurrent infections.
-
Skin Grafting: When excess or insufficient skin is an issue, skin grafting may be undertaken to restore proper penile coverage and aesthetics.
-
Surgical interventions are typically performed under general anesthesia by plastic surgeons experienced in reconstructive techniques. Each procedure is tailored to the patient's anatomical and functional needs, with post-operative care strategies designed to prevent complications and facilitate recovery. Transitioning between medical and surgical options depends on the severity of the symptoms and the patient's preferences.
A Closer Look at Hidden Penis Surgery: Procedures and Techniques
Hidden penis surgery involves specialized procedures aimed at addressing the condition where the penis is concealed beneath the skin, fat, or surrounding tissues. This condition, known as a hidden or buried penis, may result from congenital causes, obesity, trauma, or previous surgical complications. The primary goals of the surgery include restoring functionality, improving hygiene, and enhancing the patient's sexual health and self-esteem.
Several surgical techniques are employed depending on the underlying cause and severity of the condition:
- Common Procedures
- Suspensory Ligament Release.
This technique involves releasing the suspensory ligament of the penis, which attaches the penile shaft to the pubic bone. By releasing this structure, the penis can achieve greater projection, particularly in cases of tethering caused by skin or fat overgrowth.
Skin and Fat Removal
Excess fat deposits around the pubic area, often referred to as a "fat pad," can engulf the penis and contribute to its buried appearance. Liposuction or surgical excision is used to remove excess fat and ensure a reduced obstruction. Additionally, redundant skin may be trimmed or repositioned for better exposure of the penile shaft. There are two types of reductions: vertical and horizontal. During a horizontal reduction, an incision is made across the top of the pubic region. Pubic fat is directly excised, skin is lifted, resected, and tacked to close the space. There are two types of vertical reductions: lateral and central. During a lateral vertical reduction, an incision is made on each side of the penis, and the incision extends to the scrotum, resulting in two somewhat parallel scars. Alternatively, with central vertical pubic reduction, a single incision can be made in the center of the pubic region. The incision starts above the shaft of the penis and then extends down the sides of the base of the penis into the scrotum. The resulting scar resembles an upside-down letter "Y" with the base of the penis in the center. Both the lateral and central pubic reductions involve the direct excision of pubic fat, release of the suspensory ligament with the skin being pulled vertically and resected.
Z-Plasty or Other Skin Reconstruction Techniques
For cases involving severe scarring or congenital skin deformities, reconstructive techniques such as Z-plasty may be employed. These methods are designed to redistribute tension and improve functional aesthetics.
Additional Interventions:
-
Penile Degloving: This approach involves separating the skin from the shaft to realign tissue more effectively.
-
Scrotal Remodeling: If the scrotal tissue has encroached upward, reshaping it enhances the appearance and mobility of the genital area.
-
Urethral Adjustment: In certain instances, urethral repair is also performed to minimize urinary challenges stemming from buried anatomy.
The surgical process is tailored to individual needs, with detailed pre-operative assessments ensuring the most effective technique selection. These procedures are often performed under general anesthesia and require post-operative follow-up for successful outcomes.
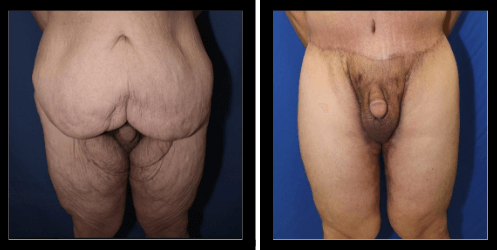
Figure #4: Case #1: 45-year-old with hidden penis. He was 5’10” and weighted 372 lbs. and lost 160lbs. with diet, exercise, and gastric bypass. He underwent horizontal reduction with an incision across the top of the pubic region. The suspensory ligaments were released. Pubic fat was directly excised, and skin lifted, resected, and tacked to close the supra-pubic space.
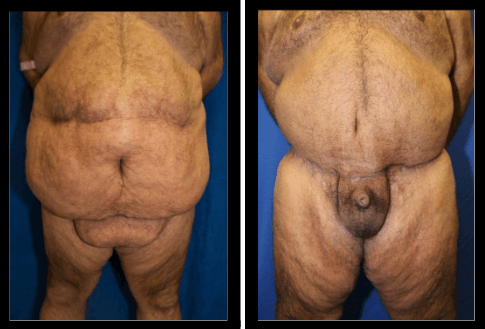
Figure #5: Case #2: This is a 45-year-old male who weighed 690 pounds. He underwent gastric bypass surgery and lost 330 pounds. He was unhappy with the excess skin and his hidden penis. He underwent a horizontal reduction with a supra-pubic incision, across the top of the pubic region. Pubic fat was directly removed. The pubic skin removed and lifted. His suspensory ligaments were released.
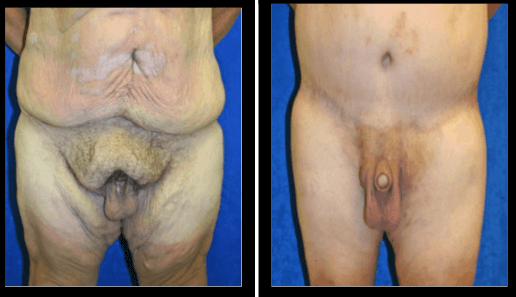
Figure #6: Case #3: 42-year-old with hidden penis. He was 5’8” and 180 lbs. Previously, he weighted 400lbs. He underwent RNY gastric bypass and lost 120lbs. he underwent a central vertical pubic reduction with an inverted Y technique. The central vertical reduction includes direct excision of pubic fat, release of the suspensory ligament and the skin being pulled vertically and resected.
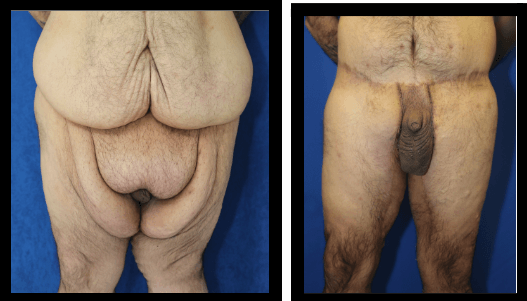
Figure #7: Case #4: A 38-year-old male, 5' 11", 295lbs. His maximum weight was 540lbs. He had lost 245lbs through diet, exercise, gastric sleeve surgery, and gastric bypass surgery. He presented with a hidden penis due to the excess skin and fat surrounding the supra-pubic region, shaft of the penis, and scrotum. The patient underwent bilateral lateral vertical pubic reduction. This included 1) superior horizontal reduction with the removal of excess skin and fat in the supra-pubic region, 2) subdermal lipectomy excision (direct removal of fat) around the base of the penis, 3) release of suspensory ligaments allowing penile lengthening, and 4) bilateral vertical reduction with the removal of excess skin and fat of the lateral pillars of the scrotum and supra-pubic region.
Recovery and Post-Surgery Care for Hidden Penis Surgery
Proper recovery and post-surgical care are essential for ensuring the success of hidden penis surgery, minimizing complications, and achieving the desired outcomes. After reconstructive plastic surgery, the patient typically remains under observation until stable and is advised on home-care protocols to promote healing.
Key components of the post-surgery recovery process include:
-
Pain Management: Discomfort and swelling are common during the initial recovery phase. Plastic surgeons usually prescribe pain relievers to alleviate symptoms.
-
Wound Care: Keeping the surgical site clean and dry is critical to prevent infection. Patients are given detailed instructions on cleaning the area and changing dressings.
-
Activity Restrictions: Physical activity, especially strenuous exercise and heavy lifting, is usually restricted for several weeks to prevent strain on the surgical site.
-
Compression Garments: Occasionally, compression garments may be recommended to reduce swelling and support the surgical area.
Follow-up appointments with the plastic surgeon are scheduled to monitor the healing process and address any concerns that may arise. Common post-operative instructions may also include avoiding smoking and adhering to a protein-rich diet to support tissue repair.
Patients are generally advised to refrain from sexual activity until the plastic surgeon confirms that healing is complete. Gradual resumption is typically encouraged under guidance to minimize disruption to sensitive tissues.
Complications such as infection, excessive bleeding, or delayed healing are rare but possible. Patients are instructed to contact their healthcare provider promptly if these occur, ensuring timely intervention.
Improvement in Sexual Health After Treatment
Hidden penis surgery often provides notable benefits in sexual health, addressing both physical and psychological aspects that previously hindered intimate relationships. The procedure typically removes excess skin and fat that obscures the penis, allowing for better external exposure. This anatomical improvement enhances the individual's ability to engage in sexual activities effectively and without discomfort. Patients frequently report increased sensation, which can positively impact sexual performance and satisfaction.
Additionally, the surgery alleviates common complications related to penile concealment, such as inflammation, recurring infections, and discomfort during intimate moments. By improving hygiene and reducing the risk of infection, the procedure fosters a healthier environment around the genital region, thereby minimizing barriers to physical intimacy. The elimination of physical pain or irritation during intercourse often encourages individuals to feel more confident in pursuing sexual relationships.
Psychologically, the surgery can lead to an improvement in self-esteem and body image. Many individuals with a hidden penis experience feelings of inadequacy or shame that can negatively affect their sexual confidence and emotional intimacy. Post-treatment, a significant number of patients report experiencing relief from these emotional burdens, aiding in the restoration of their sexual identity. This newfound confidence supports healthier encounters and partnerships, as patients feel less inhibited and more willing to explore their sexuality.
Post-operative care also plays a key role in sustaining sexual health improvements. Patients are advised to follow rehabilitation protocols, maintain proper hygiene practices, and consult healthcare providers for guidance throughout their recovery. Observing these measures ensures long-term benefits, allowing patients to embrace their renewed physical abilities while fully safeguarding their sexual well-being.
Lifestyle Changes and Preventive Measures for Long-Term Care
Adopting lifestyle changes alongside preventive measures can greatly support the outcomes of hidden penis surgery, enhancing hygiene, reducing the risk of infections, and promoting sexual health. These strategies complement surgical intervention by ensuring optimal recovery and minimizing complications.
-
Healthy Weight Management: Maintaining a healthy weight is crucial in supporting the long-term success of hidden penis surgery. Excess body fat, particularly around the pelvic and groin areas, can contribute to the recurrence of tissue folding or pressure that exacerbates the hidden condition. Incorporating balanced dietary practices, such as consuming nutrient-dense meals, limiting processed foods, and monitoring caloric intake, can help stabilize weight. Regular physical activity, including resistance training and cardio exercises, can improve muscle tone and circulation, benefiting overall health.
-
Skincare and Hygiene Practices: Proper hygiene and skincare routines prevent infections and enhance post-surgical comfort. Patients are encouraged to clean and dry the groin area, using mild soaps that avoid irritation. If your plastic surgeon recommends, applying talcum powder or antifungal creams can further reduce moisture buildup and bacterial growth. Equally important is wearing breathable and loose-fitting underwear to prevent chafing in the surgical area.
-
Sexual Health Awareness: Promoting sexual health through open communication with healthcare providers can help address concerns tied to confidence, sensation, or functionality post-surgery. Regular screenings for sexually transmitted infections (STIs) and practicing safe sex are encouraged as part of preventive care. Addressing psychological aspects such as self-esteem or body image concerns can play a significant role in restoring sexual well-being.
-
Routine Medical Follow-Ups: Regular consultations with medical professionals are key in identifying complications early and ensuring proper healing. Plastic surgeons may recommend periodic examinations to assess progress, manage scar tissue, or address residual conditions. Patients are advised to promptly report any unusual symptoms, such as persistent pain, swelling, or discharge, to their healthcare team.
-
Avoiding Risk Factors: Minimizing exposure to risk factors such as smoking or alcohol intake can enhance recovery and safeguard overall wellness. Smoking impairs circulation and slows wound healing, which may negatively affect the surgical site. Developing a plan to quit smoking or reduce alcohol consumption gradually can be beneficial for long-term health maintenance.
FAQs About Hidden Penis Surgery and Related Conditions
-
What is hidden penis surgery? Hidden penis surgery is a medical procedure designed to correct buried or concealed penises, often caused by factors such as excess fat in the pubic area, scar tissue, or skin conditions. The surgery aims to restore normal penile appearance, improve hygiene, reduce infections, and address sexual health concerns.
-
Who is a candidate for this surgery? Candidates typically include individuals experiencing difficulty with hygiene, recurrent infections, or impaired sexual function due to a hidden penis. A thorough evaluation by a plastic surgeon determines eligibility based on physical condition, underlying causes, and overall health.
-
What risks are associated with this procedure? As with any surgery, risks include infection, bleeding, scarring, and possible recurrence of the condition. Some individuals may also experience changes in penile sensation or dissatisfaction with aesthetic results. Discussing risks with a qualified specialist is crucial.
-
How is the recovery process? Recovery varies depending on surgical complexity and individual factors. Typically, patients can resume light activities after a few weeks but may need several months for full healing. Follow-up visits ensure proper recovery and address any complications that may arise.
-
Does hidden penis surgery impact sexual function? The surgery often improves sexual function by enhancing exposure and addressing physical or psychological barriers. However, outcomes depend on the patient's baseline condition and the specific surgical techniques employed.
-
Are there alternatives to surgery? Non-surgical options may include weight loss, physical therapies, or devices to manage fat distribution or skin conditions. These methods are typically less effective for severe cases, but can be helpful in specific circumstances.
-
What costs are involved? Costs vary based on the complexity of the surgery, the expertise of the plastic surgeon, and the geographic location. Health insurance may partially cover the procedure if deemed medically necessary.
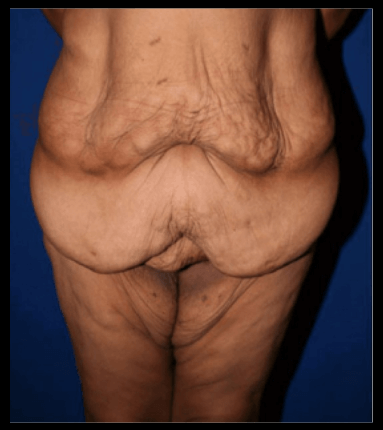
Figure 8: Obesity and significant weight loss can contribute to hidden penis
Conclusion: Finding Solutions for Improved Quality of Life
Addressing the challenges associated with hidden penis conditions requires a multidisciplinary focus, involving medical, psychological, and lifestyle interventions. Surgical treatments, often involving corrective procedures to release buried and obscured penile tissue, are crucial in improving functional and aesthetic outcomes. These surgeries aim to decrease complications such as recurrent infections, difficulty maintaining hygiene, and impairments in sexual health.
Post-surgical care is essential to ensure success and prevent complications. Post-operative care often entails personalized aftercare plans, including wound management, monitoring for signs of infection, and adherence to prescribed medications or topical treatments. Patients are often encouraged to work closely with their plastic surgeons to optimize recovery and maintain the long-term benefits of the surgery.
While surgery is a significant component of treatment, non-surgical measures can also enhance overall outcomes. Weight management programs can be particularly beneficial for individuals struggling with obesity-related hidden penis conditions, as excess fat tissue in the pubic area often exacerbates the problem. Psychological counseling may also be necessary to address self-esteem issues or emotional distress stemming from the condition.
Healthcare professionals emphasize the importance of patient education, equipping individuals with knowledge to make informed decisions about their care. Awareness campaigns and tailored consultations can reduce stigma and improve access to effective treatment options. By combining medical interventions, lifestyle modifications, and education, individuals can achieve improved hygiene, reduced infection risks, and a more fulfilling sexual life.
Achieving sustainable improvements in quality of life depends on a patient-centered approach that incorporates both physical and emotional well-being. This approach acknowledges the complexities of the condition, fosters open communication, and prioritizes long-term health and well-being.

Figure 9: Dr. Katzen’s Beverly Hills office at 9735 Wilshire Boulevard, Suite 407, Beverly Hills, CA 90212
If you or someone you know has a hidden penis and wishes consultation for correction, please get in touch with Dr. J. Timothy Katzen at (310) 850-7770 or email scheduling@timothykatzenmd. Dr. Katzen can meet with you in his office located in Beverly Hills. Alternatively, Dr. Katzen can arrange a virtual consultation on Zoom, Skype, FaceTime, and WhatsApp.