The Comprehensive Guide to Widened, Hypertrophic, and Keloid Scars
11/2/2025
Scars develop as a natural component of the body’s healing process when the epidermis restores itself following injury, trauma, or plastic surgery. Scar formation entails the synthesis of collagen, a protein that reinforces the integrity of the incision site. The morphology and features of a scar can be influenced by multiple factors, including the type of injury, the individual’s healing process, genetics, and external factors such as infection, the presence of foreign bodies like silicone or sutures, or inadequate wound management. Various varieties of scars exist, each possessing unique features and underlying etiologies.
How The Body Naturally Forms Scars:
A scar on the skin is the result of healing from trauma to the skin. There are four distinct stages of initial healing following an injury: hemostasis, inflammation, proliferation and remodeling.
The first stage of normal wound healing is hemostasis, which means stopping the bleeding. The main cells and molecules involved are platelets, fibrin, and proteoglycans.
The second phase of normal wound healing is the inflammatory phase. During the inflammatory phase, blood vessels supply the essential cells to the site of trauma. Specialized cells include macrophages, neutrophils, and lymphocytes. Macrophages are like a little Pac Man that eats away devitalized tissue and facilitate tissue repair. During this initial phase, the body constructs a transient scaffold composed predominantly of type III collagen.
?The third phase of normal wound healing is called the granulation and proliferative phase. The granulation and proliferative phase is highlighted by the fibroblast. Fibroblasts are like little muscle cells. Fibroblasts deposit a temporary collagen matrix and provide structural support to the wound. During this phase, type III collagen is the predominant collagen deposited and is arranged in a disorganized and irregular manner. By contracting, the fibroblasts also facilitate the contraction of the wound. Also, new blood vessels are formed and deliver oxygen to the regenerating cells. The wound begins to become covered with epithelial and endothelial cells.
The last stage of wound healing encompass maturation and remodeling, during which the wound continues to heal. The body replaces less resilient collagen type III with a more robust and stronger type I collagen. Throughout scar maturation, collagen type III is replaced by collagen type I. Gradually, collagen type I becomes the predominant collagen, and the fibers are cross-linked and organized to develop a durable and mature scar. This collagen replacement procedure is carried out over a period of up to two years with the aim of reinstating strength and flexibility. However, even at two years post-injury, a fully healed scar generally exhibits approximately 70 to 80% of the tensile strength of the original, uninjured epidermis. This scar tissue will not fully recover the original tissue's strength or flexibility.
Typical Varieties of Scars

Figure #1: Picture of widened scars on a female abdomen after massive weight loss. Scars are flat, depressed or recessed and are limited to the borders of the scar. Created by CHATGPT on 10/10/2025.
1. Widened scars (atrophic or stretch scars): These scars occur due to insufficient collagen synthesis during the healing process, resulting in a depressed or recessed appearance. Common examples include scars associated with acne, chickenpox, or rapid skin stretching during periods of weight gain, muscle bulking, or pregnancy.
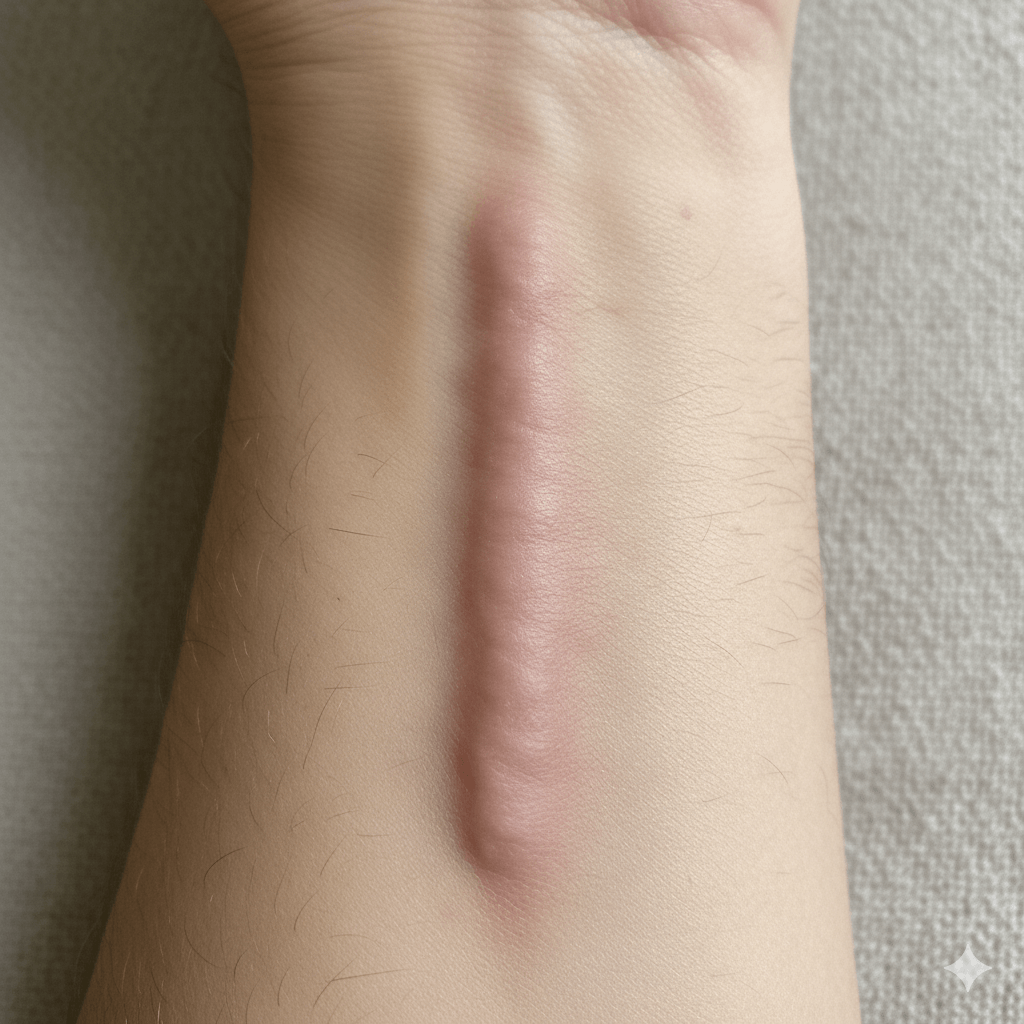
Figure #2: Picture of a hypertrophic scar with mildly elevated, pink scar. Created by Gemini on 10/13/2025.
2. Hypertrophic Scars: These scars are distinguished by their elevated, erythematous (red or pink) appearance. Hypertrophic scars develop as a result of excessive collagen synthesis contained within the confines of the original incision. These scars frequently form following burns, surgical incisions, or trauma and may naturally diminish over time without the need for targeted intervention.
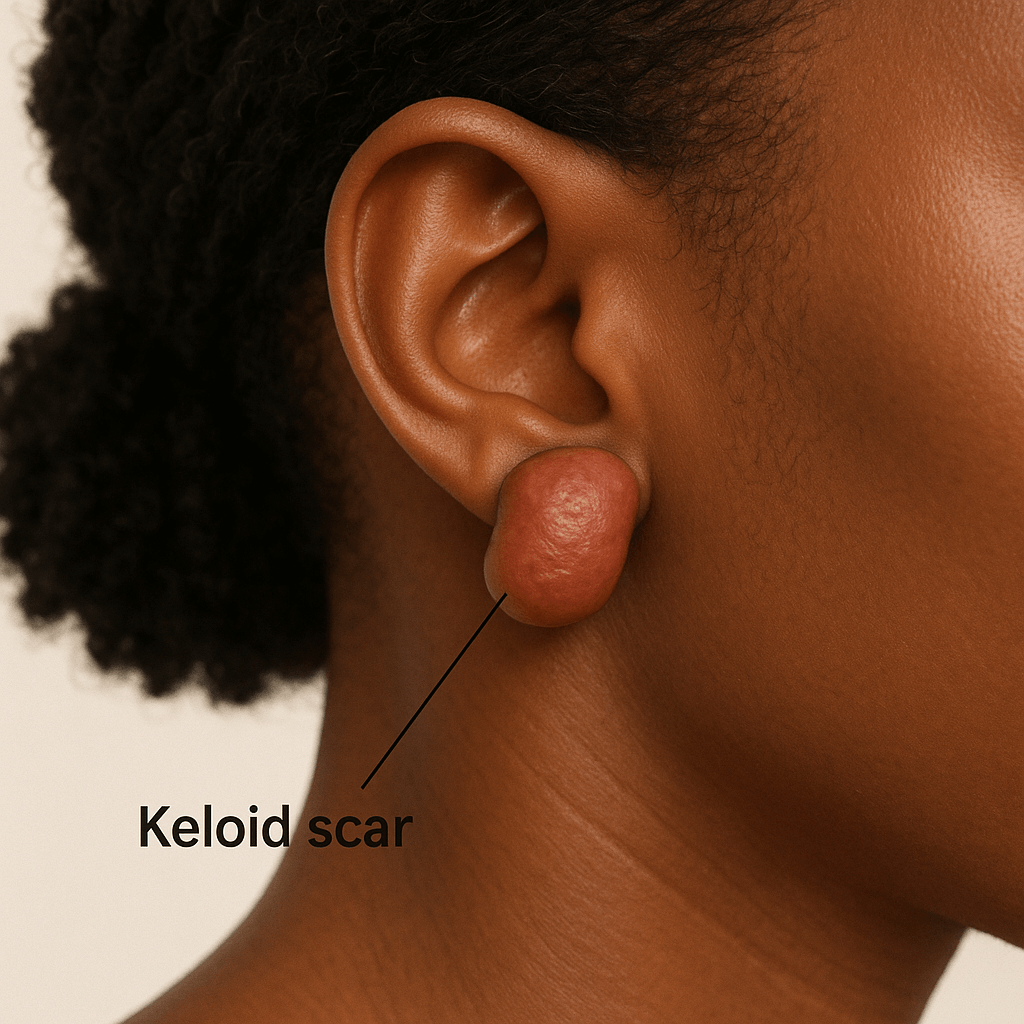
Figure #3: Picture of a keloid scar on the front of a patient's earlobe. Keloids are often raised, outgrow the normal borders of a scar, and are more common in darker pigmented patients. Keloids have a family history. Created by CHATGPT 10/10/2025.
3. Keloid Scars: Keloids are raised, hypertrophic scars that extend beyond the original incision margins, resulting from an exaggerated response during the skin’s healing process. Factors including genetic predisposition, darker skin pigmentation, and skin trauma such as piercings or surgical procedures may elevate the risk of keloid development.
Factors Affecting Scar Formation
Multiple factors influence the formation and extent of scarring:
1) Injury Type and Severity: Deep wounds or burns are more prone to result in conspicuous scarring.
2) Genetics: Certain individuals possess a genetic predisposition to develop hypertrophic or keloid scarring.
3) Wound healing conditions: Inadequate hydration, infection, and exposure to ultraviolet rays may exacerbate scar formation.
4) External Stress: Applied pressure on regenerating skin may result in the expansion of scars.
Comprehending these scar classifications and their origins is crucial for identifying suitable preventive strategies and therapeutic interventions.
Understanding Widened Scars: Features and Development
Widened scars, also known as atrophic linear scars, develop when healing skin is subjected to excessive tension or stretching. These scars are characterized by a flat and pale appearance, typically broader than the initial incision. In contrast to hypertrophic or keloid scars, widened scars do not encompass elevated or thickened tissue. Instead, they are distinguished by their expansive, smooth surface and may develop a shallow depression at the location of the healing wound.
A significant factor influencing their development is the tension exerted on the wound margins throughout the healing process. Wound tension may arise from movement in highly mobile regions, such as the knees, shoulders, abdomen, or from inadequate support, such as the use of insufficient sutures during surgical procedures. Skin elasticity and comprehensive wound management also serve important functions. Individuals with sensitive or thin skin, such as elderly individuals or those affected by connective tissue disorders, may have a higher susceptibility to developing hypertrophic scarring.
Widened scars are frequently linked to surgical incisions but may also arise from injuries, fires, or other forms of trauma. Generally, widened scars develop when the dermis produces insufficient collagen to approximate the incision edges effectively. External forces, such as tension or elongation of the epidermis during the healing process, further increase their likelihood.
Over time, expanded scars may become flatter and less prominent, but they seldom completely dissolve. The final appearance of the scar may differ based on the scar’s position, length, and breadth. In certain instances, scars may be accompanied by irritation or discomfort; however, these scars generally do not cause sensitivity or pain. Proper wound management, including consistent hydration, pressure therapy, and silicone gel treatments, can diminish the prominence of the scar and enhance overall healing results. Timely intervention during the healing process is essential for reducing the extent of scar enlargement.
What Is the Nature of Hypertrophic Scars?
Hypertrophic scars are a particular form of scar that develops as part of the skin’s innate healing response after injury, surgery, or trauma. These scars are distinguished by their elevated and hypertrophic appearance, resulting from excessive collagen synthesis during the wound healing process. Unlike typical scars, hypertrophic scars are limited to the site of the initial injury or incision and do not extend into the adjacent epidermis.
Hypertrophic scars typically form within several weeks following skin injury. They are most frequently observed in regions of the body subject to tension, such as the chest, upper back, shoulders, and joints. They may differ in color and texture, presenting shades of pink or red, and feeling firm when touched. Although they may diminish over time, hypertrophic scars generally do not resolve completely without intervention.
Numerous factors play a role in the development of hypertrophic scarring. These factors encompass the depth and severity of the injury, genetic predisposition, inadequate wound management, and environmental factors such as infection or recurrent friction on the afflicted region. Certain individuals, especially those with darker skin tones, are more susceptible to developing hypertrophic scarring owing to variations in collagen production and skin healing mechanisms.
Hypertrophic scars frequently present with physical symptoms, including pruritus (itchiness), tenderness, or restricted mobility in regions adjacent to joints. They may also exert a psychological effect, inducing distress in affected individuals because of their conspicuous appearance.
Treatment modalities for hypertrophic scars differ based on the severity of the condition and patient preferences. These options can include silicone sheeting or gels, corticosteroid injections, laser treatment, or surgical procedures. Addressing these scars frequently requires a combination of treatments designed to diminish their appearance and enhance the skin’s texture in the affected areas.

Figure #4: Thick, raised, red keloid scar over shoulder. Keloids are more common in high mobility joints, like the shoulder and knee. Created by CHATGPT on 10/10/2025.
Keloid A Comprehensive Examination of Keloid Scars
Keloid scars denote a form of abnormal wound recovery characterized by the excessive proliferation of scar tissue that extends beyond the original injury boundaries. Characterized by their elevated and hypertrophied appearance, keloids can develop as a result of various skin injuries, such as surgical incisions, acne, piercings, burns, insect bites, and vaccinations.
Unlike hypertrophic scars, keloids have the capacity to continue enlarging over time rather than reaching a stable size or diminishing. They are frequently smooth, glossy, and resilient to the touch, exhibiting a color spectrum that spans from pink and red to dark brown, contingent upon the individual’s skin tone. Keloids are not confined to a specific region but most frequently develop on the chest, shoulders, earlobes, jawlines, and upper back.
Research indicates that the development of keloids is affected by a combination of genetic susceptibility, skin tension, and the inflammatory response to cutaneous injuries. Individuals with darker skin complexions, including those of African, Hispanic, or Asian heritage, demonstrate a greater propensity for developing keloids relative to individuals with paler skin tones. Furthermore, keloids are more commonly observed in younger populations, especially between the ages of 10 and 30.
Symptoms of keloids go beyond their aesthetic appearance. Many individuals afflicted report experiencing itching, tenderness, or even pain associated with the scar tissue. These symptoms can significantly impact an individual’s emotional well-being and self-esteem, particularly when the keloid develops in visible areas.
Management of keloid scarring encompasses a range of approaches, including corticosteroid injections, cryotherapy, silicone gel sheets, and pressure therapy. Other medical interventions, including laser therapy, surgical excision, or radiation treatment, are used for keloid cases that are refractory or persist. Typically, preventing keloid formation necessitates proactive measures, including refraining from unnecessary piercings and effectively managing incisions to reduce inflammation.
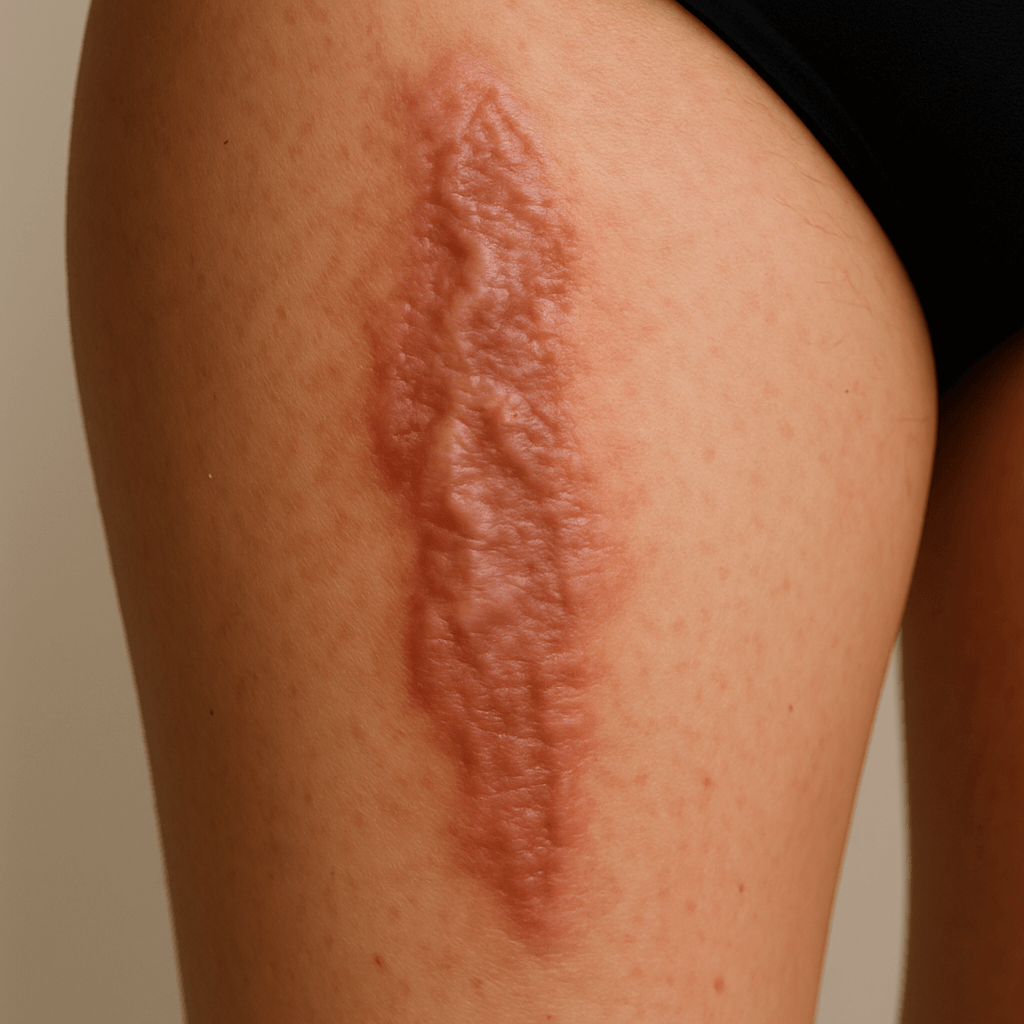
Figure # 5: Picture of a chemical burn scar to anterior right thigh. Wound classification is important for treatment protocols. Created by CHATGPT on 10/10/2025.
Differences Among Widened, Hypertrophic, and Keloid Scars
Widened, hypertrophic, and keloid scars vary in their morphology, development process, and therapeutic strategies. Comprehending these distinctions is vital for their accurate identification and effective management.
1. Widened Scar Tissue
Widened scars generally arise from tension exerted on a healing wound, which hinders the proper approximation of wound boundaries. These scars frequently present as elongated and flattened, seamlessly blending with the surrounding epidermis but extending beyond the original wound area. These scars are frequently observed following surgical incisions or inadequately supported wound closures. Unlike hypertrophic and keloid scars, widened scars are less elevated or thickened, rendering them more subtle yet potentially conspicuous due to their size and integrating qualities. They typically do not extend beyond the perimeter of the original lesion.
2. Hypertrophic Scars
Hypertrophic wounds are distinguished by an abnormal overproduction of collagen during the healing process. They are red, elevated, and may feel firm upon palpation. Nevertheless, they continue to be restricted to the location of the initial injury. Causes include trauma, burns, or plastic surgical interventions characterized by excessive healing responses. Hypertrophic lesions may undergo spontaneous improvement over time, frequently flattening and diminishing in redness as collagen fibers realign. Factors such as the severity and site of injury affect their development; however, they are typically less aggressive than keloid scars.
3. Keloid Hypertrophic Scars
Keloid scars are characterized by an excessive proliferation of fibrous tissue, resulting in elevated, distended regions that extend beyond the original wound margins. They are generally more pigmented or exhibit a pinkish hue in comparison to the adjacent skin, with variations depending on the individual’s complexion. Keloids frequently arise from a genetic predisposition and are more prevalent among individuals with darker skin tones. These wounds are prone to persistent growth and do not tend to flatten spontaneously. Although keloids may induce distress, itching, and pain, keloids often present cosmetic issues owing to their size and prominence.
Differentiating these wounds necessitates careful examination of their appearance, boundaries, and progression. Identifying these characteristics can inform suitable treatment or management strategies.
Common Risk Factors Contributing to Scar Formation
Scars develop as a natural component of the body’s wound-healing process; however, specific factors can elevate the risk of forming widened, hypertrophic, or keloid scars. These risk factors may be inherent, about an individual’s attributes, or external, influenced by environmental or contextual factors.
1. Intrinsic Elements

Figure #6 : Genetics play a critical role in the final appearance of a scar. Created by CHATGPT on 10/13/2025.
A. Genetics: Some individuals may possess a hereditary predisposition to forming abnormal scarring, such as keloids. Research suggests that keloids are more frequently observed in individuals with darker skin complexions, including those of African, Hispanic, or Asian heritage.
B. Age: skin elasticity and collagen composition change with age. Younger individuals, especially those aged between 10 and 30 years, tend to be more susceptible to aggressive scarring, such as hypertrophic and keloid scars, due to heightened collagen synthesis.
C. Hormonal Influence: Fluctuations in hormone levels, such as those occurring during pregnancy or puberty, can impact the skin’s healing process, rendering the wound more vulnerable to the development of abnormal scarring.
D. Underlying Medical Conditions: Chronic illnesses such as diabetes, autoimmune diseases, or weakened immune systems may impede effective wound healing, thereby elevating the likelihood of problematic scarring.
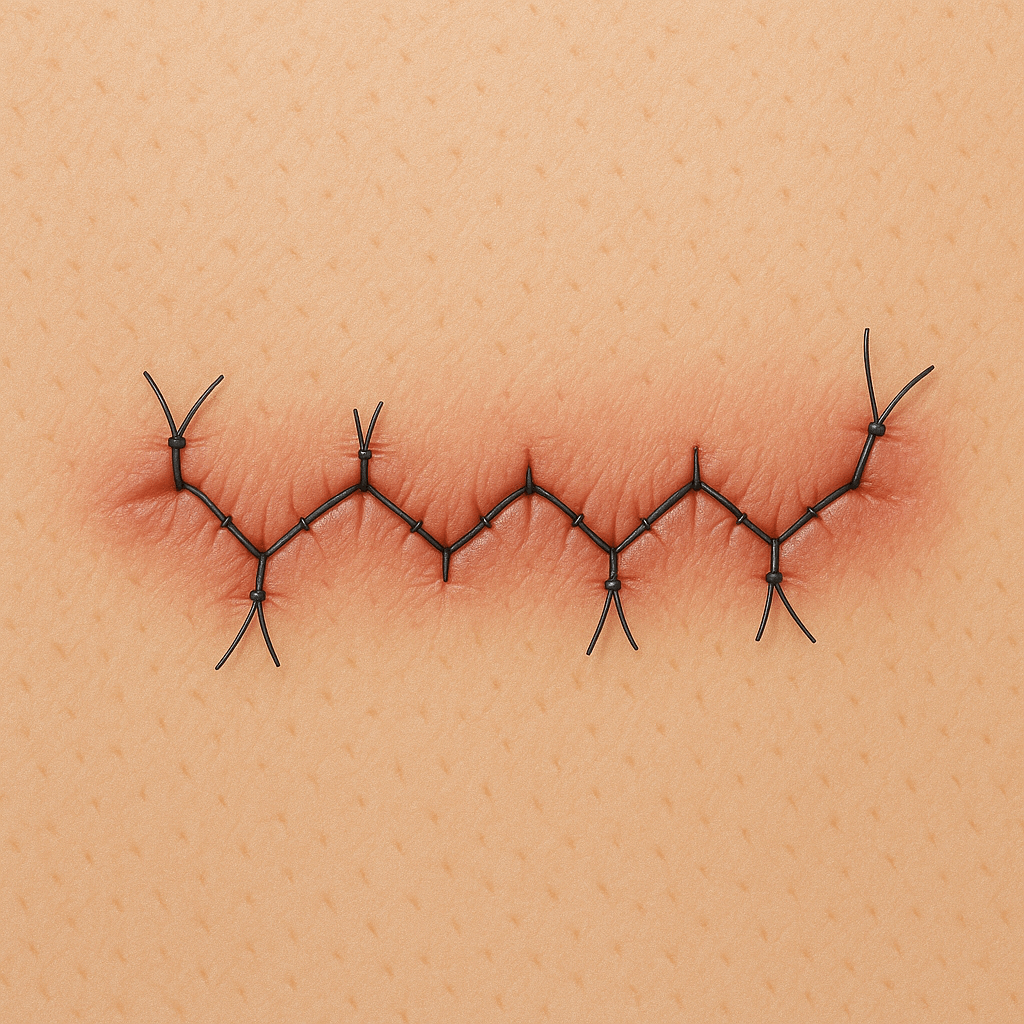
Figure #7: Picture of a jagged wound closure. Resulting scars from wound closure depend on infection, tension, wound care, and exposure to secondhand smoke. Created by CHATGPT on 10/10/2025.
2. External Influences
A. Excessive tension surrounding a wound can cause the epidermis to separate, leading to the formation of widened scars. This phenomenon is especially prevalent in incisions situated in regions of high mobility, such as the knees or shoulders.
B. Infections or delayed healing impair the organized synthesis of collagen, increasing the risk of hypertrophic or keloid scar formation.
C. Inadequate wound care, including neglecting to clean or moisturize the affected area, can worsen inflammation and influence the final appearance of the scar.
D. Wound scars located over regions with denser skin or greater tension, such as the chest, upper back, or joints, are more prone to developing as hypertrophic or keloid scars.
E. Secondhand smoke can impair wound healing and the subsequent development of thick scars.
Comprehending these risk factors facilitates the identification of individuals at increased risk of developing hypertrophic or raised scarring, thereby supporting targeted preventive and management approaches.
Diagnosis and Assessment of Scar Classifications
Comprehending the classification of the scar is crucial for establishing suitable treatment approaches. A comprehensive diagnosis necessitates the assessment of multiple clinical and patient-reported factors, including the scar’s anatomical characteristics, associated symptoms, and the scar’s developmental history. Plastic surgeons employ a combination of visual evaluation, palpation, and medical history to categorize scars as widened, hypertrophic, or keloid.
1. Visual Examination and Palpation
During the visual assessment, the scar’s size, shape, color, and texture are meticulously evaluated. Widened scars generally manifest as flat, stretched markings and may not exhibit the elevation observed in hypertrophic and keloid scars. Hypertrophic scars are limited to the borders of the initial incision and typically display elevated, firm, and erythematous features. Conversely, keloid scars surpass the boundaries of the original incision and frequently exhibit uneven, bulbous protrusions. Palpation is employed to evaluate the firmness of the scar, its adherence to underlying tissues, and the degree of fibrosis.
2. Patient-Centered Considerations
The chronology of scar formation serves as a vital diagnostic instrument. Hypertrophic scars typically manifest within weeks following injury, whereas keloids generally require a lengthier period to develop. Patients may report symptoms such as pruritus, tenderness, or pain, which are prevalent in both hypertrophic and keloid scars but less prominent in widened scars. Family history of keloids, darker skin pigmentation, and previous occurrences of aberrant scarring are also important factors to consider, as they increase the likelihood of keloid development.
3. Clinical Instruments and Technologies
Advanced diagnostic instruments serve a supplementary function. Dermoscopy facilitates improved visualization of the scar’s vascular features, pigmentation, and surface characteristics. Ultrasound imaging, especially high-frequency devices, is frequently utilized to evaluate scar thickness and alterations in underlying tissues. For research purposes, instruments such as the Vancouver Scar Scale (VSS) or the Patient and Observer Scar Assessment Scale (POSAS) are utilized to evaluate scar severity objectively. These measures distinguish between the functional and aesthetic effects of distinct scar types.
Therapeutic Approaches for Enlarged Scars
Widened scars, frequently caused by tension during wound healing or inadequate wound closure, can affect both aesthetic appeal and self-esteem. Treatment seeks to reduce their visibility and enhance skin texture. A range of approaches is available, each customized to the individual’s particular requirements, scar features, and medical background.
1. Non-Invasive Therapeutic Approaches: Non-invasive therapies are frequently the initial approach and may prove effective in specific situations:
A. Silicone Products: Silicone sheeting and gels are widely used to reduce the size and discoloration of scars. Silicone may assist in hydrating the epidermis and in regulating collagen synthesis.
B. Topical Treatments: Over-the-counter or prescription formulations incorporating constituents such as retinoids, onion extract, or vitamin E may assist in enhancing the scar’s appearance over time.
C. Steroid Injections: Administration of corticosteroid injections can diminish inflammation, smooth the scar, and enhance elasticity in specific widened scars.
2. Minimally Invasive Surgical Procedures: When non-invasive techniques fail to produce the desired outcomes, minimally invasive procedures may be utilized to address underlying scar tissue.
A. Microneedling: This technique involves creating micro-injuries to stimulate collagen remodeling, thereby improving the texture and density of the widened scar.
B. Laser Therapy: Laser procedures, including fractional CO2 laser or pulsed dye laser, can improve skin tone, diminish erythema, and refine the surface of the scar.
C. Dermal Fillers: Injectable agents can effectively replenish volume in scars that are recessed or indented.
3. Surgical Reassessment: For extensively widened scars, surgical procedures may be advised:
A. Scar Revision surgery: This procedure eliminates the widened scar and repositions the epidermis to facilitate improved healing. Appropriate post-operative care reduces the likelihood of recurrence.
B. Z-Plasty or W-Plasty: These techniques modify the direction of the scar to harmonize with the natural skin lines, enhancing its aesthetic appearance.

Figure #8: Picture of scar reconstruction with a Z-plasty. Plastic surgeons use Z-plasty techniques to decrease the tension in a scar. Created by CHATGPT on 10/10/2025.
Integrated Methodologies
A. In some instances, a combination of treatments yields the most optimal outcomes. For example, surgical revision may be succeeded by laser therapy or silicone application to enhance the healing process.
B. Consultation with a plastic surgeon is essential for identifying the most appropriate treatment plan and attaining optimal results.
Managing and Minimizing Hypertrophic Scars
Hypertrophic scars, distinguished by their elevated and erythematous appearance, develop due to excessive collagen synthesis during the process of wound recovery. Managing and minimizing these lesions requires a combination of preventive measures, medical treatments, and at-home care protocols.
1. Preventive Strategies: To effectively manage hypertrophic scarring in its early stages, it is essential to initiate preventive measures promptly once wound healing commences.
2. Proper Wound Care: Gently cleanse the wound frequently with mild detergent and water to prevent infection and facilitate optimal healing. Moisturization and Dressing: Maintain hydration of the area with approved ointments and protect it with non-stick, breathable dressings or silicone sheeting.
3. Minimizing Tension: Refrain from engaging in activities that impose excessive strain on the laceration to prevent overstretching of the tissue. This includes exercising and stretching.
Local Therapeutic Applications
Numerous over-the-counter and prescription topical therapies may assist in the reduction of hypertrophic scars:
- Silicone-Based Products: Silicone gels and sheeting are commonly advised due to their ability to hydrate the skin and modulate collagen synthesis.
- Onion extract gels: Certain gels containing onion extract may help gradually reduce scar thickness.
- Steroid creams: Corticosteroid-based formulations are efficacious in diminishing erythema and inflammation linked to hypertrophic scars.
Medical Procedures
For more prominent hypertrophic scarring, medical interventions may be utilized:
- Corticosteroid Injections: These injections diminish inflammation associated with scars and help flatten elevated tissue.
- Laser Therapy: Laser procedures can enhance the coloration and surface quality of scars by addressing hyperpigmented regions.
- Surgical Revision: In critical cases, surgical interventions may be performed to excise or modify the affected tissue.
Lifestyle Modifications
- Sun Protection: Ultraviolet exposure may exacerbate scar discoloration. Applying sunscreen with a high SPF is imperative.
- Healthy Nutrition: A diet abundant in vitamins C and E, along with zinc, may promote the healing process.
- Avoid Smoking: Tobacco hinders circulation and impedes the healing process of scars.
With careful attention, the appearance of hypertrophic scars can improve markedly over time.
Effective Therapeutic Strategies for Keloid Scars
Keloid scars, distinguished by their elevated and hypertrophic appearance, frequently necessitate specialized interventions owing to their propensity to extend beyond the initial site of injury. Numerous treatment modalities are available to address keloids and enhance their aesthetic appearance. Although complete eradication is not always achievable, the objective is to diminish their size, alleviate symptoms, and restore the skin’s natural texture.
Non-Invasive Therapeutic Options
Corticosteroid Injections: Corticosteroids, administered directly into the keloid tissue, can assist in decreasing inflammation and suppressing excessive collagen synthesis, resulting in gradual scar flattening. Multiple treatment sessions are generally necessary to achieve optimal outcomes. Silicone sheets or gels: The application of silicone-based products can soften keloids, enhance their appearance, and reduce irritation. These are most effective when applied consistently over a period of several months.
- Cryotherapy: Applying liquid nitrogen to freeze the keloid can reduce the tissue size, particularly in smaller lesions. This approach is frequently combined with other therapies to achieve improved results.
- Pressure Therapy: Pressure garments apply consistent pressure to the scar, which can decrease blood flow and inhibit additional keloid development. This method is frequently employed for covering scars that span extensive areas of the body.
Sophisticated Medical Techniques
- Laser Therapy: Pulsed dye lasers or fractional laser technology can precisely target the blood vessels supplying keloids, thereby diminishing erythema and facilitating collagen remodeling. This treatment is often administered in conjunction with corticosteroid therapy to achieve a more pronounced effect.
- Radiation Therapy: Administering low-dose radiation, typically following the surgical excision of the keloid, can reduce the likelihood of recurrence by inhibiting the reformation of scar tissue.
- 5-Fluorouracil (5-FU) and Bleomycin: These chemotherapeutic agents, when administered via injection into keloids, have the capacity to diminish their size and relieve associated symptoms such as pruritus. 5-FU decreases DNA synthesis in fibroblasts. Fibroblast contribute to wound contracture. 5-FU also decreases collagen production. These injections are generally used for thick hypertrophic or keloid scars.

Figure #9: Picture of 5-FU being injected into a scar. 5-FU decreases reduces collagen production. Created by CHATGPT 10/10/2025.
Surgical Procedure
Surgical removal of a keloid may be indicated for extensive or prominent wounds that have not responded to alternative therapies. Surgical intervention alone is not advised owing to the substantial risk of recurrence. Integrating surgical procedures with supplementary treatments, including radiation therapy or corticosteroid injections, can markedly enhance success rates.
Emerging Alternatives and Lifestyle Adjustments
Emerging technologies, such as microneedling combined with platelet-rich plasma (PRP) and immunomodulators like imiquimod, demonstrate potential in the management of keloids. Ensuring appropriate wound management throughout the healing process, minimizing excessive tension on the skin, and shielding scars from ultraviolet radiation are essential measures to prevent the recurrence or exacerbation of keloids.
Home Remedies and Non-Invasive Techniques for Scar Treatment
Managing enlarged, hypertrophic, or keloid scars typically begins with readily available home remedies and non-invasive treatments that can provide relief and improve the cosmetic appearance of scars. These methods are particularly beneficial during initial phases or serve as supplementary options alongside professional interventions.
Local Therapeutic Applications
- Silicone Gel or Sheets: Silicone-based products are widely recognized for their effectiveness in reducing lesion size, pigmentation, and rigidity. When used consistently, silicone sheets form a protective barrier that maintains moisture in the scar tissue, thereby decreasing excessive collagen production.
- Vitamin E: Although its efficacy is subject to ongoing debate, Vitamin E oil is frequently utilized on scars to promote skin regeneration and reduce harshness. It is imperative to assess for skin sensitivities before extended use.
- d Due to its inherent moisturizing and antibacterial characteristics, unprocessed honey may assist in softening scar tissue gradually. Applying it as an overnight mask or combining it with other natural ingredients can provide supplementary skin benefits.
Massage and Pressure Therapy
Scar massage, when performed with gentle to moderate pressure, can enhance blood circulation and facilitate the breakdown of fibrous tissue beneath the epidermis. Consistently massaging the afflicted region with an oil or cream markedly facilitates the flattening of hypertrophic or keloid scars. Compression garments frequently fulfill a comparable role for scarring on extensive areas of the body by alleviating tension within the adjacent tissues.
Natural Oils and Gels
- Aloe Vera: Recognized for its soothing and anti-inflammatory properties, aloe vera gel may assist in calming scarred tissues and moisturizing the epidermis. Consistent application may facilitate the healing process, especially for new wounds.
- Rosehip Seed Oil: Rich in essential fatty acids and vitamins, this oil supports skin regeneration, diminishes discoloration, and refines scar texture.
Lifestyle Modifications
- Hydration and Nutrition: Consuming adequate amounts of water and adhering to a diet abundant in vitamins A, C, and E support skin elasticity and the maintenance of collagen equilibrium.
- UV Protection: Scars are especially vulnerable to sun exposure, which may exacerbate discoloration. Applying sunscreen daily provides effective protection and diminishes the likelihood of hyperpigmentation.
These methods necessitate perseverance and sustained effort over time to achieve observable progress.
When to Consult a Plastic Surgeon Regarding Scars
Recognizing the appropriate circumstances to consult a plastic surgeon regarding wounds is crucial, particularly when self-care interventions do not produce adequate outcomes. Scars, whether widened, hypertrophic, or keloid, may differ in severity and influence both physical appearance and emotional health. Understanding the indicators that necessitate professional intervention is essential for individuals managing problematic scarring.
Certain Situations That May Require Professional Assistance:
- Persistent Pain or Discomfort: If a scar results in continuous pain, irritation, or a stinging sensation that persists over time, it may necessitate medical assessment.
- Limited Range of Motion: Scars located near joints or regions of frequent movement, such as the hands or neck, may result in restricted mobility and require specialized intervention to regain functionality.
- Rapid Progression: Keloid scarring, in particular, may enlarge progressively over time. A plastic surgeon should evaluate any abrupt or swift enlargement of a scar.
- Infection or Inflammation: Signs of infection may include redness, edema, warmth, or discharge originating from a scar. Medical treatment is essential in these situations to avert potential complications.
- Psychological Distress: When a scar substantially affects self-esteem or mental health, seeking guidance from a qualified professional for appropriate treatment or counseling may enhance emotional well-being.
Standard Treatments Provided by Professionals:
- Corticosteroid Injections: Frequently employed in the treatment of hypertrophic and keloid scarring to diminish inflammation and reduce their size.
- Laser Therapy: Improves skin texture and pigmentation to enhance the appearance of the scar.
- Surgical Revision: Intended to re-excise extensive wounds or to rectify abnormal healing processes.
- Cryotherapy: A suitable treatment for smaller keloids, employing freezing procedures to reduce their size.
Promptly obtaining professional assistance can avert additional complications and facilitate optimal recovery.
Strategies for Preventing Scar Formation
Reducing the risk of scar formation necessitates a proactive strategy throughout the wound healing process. Appropriate care and prompt interventions are vital to promote optimal skin healing and minimize abnormalities in scar tissue.
Prompt Wound Management
- Promptly cleanse the wound: Gently rinse the affected area with clean water to eliminate debris and bacteria. Apply a mild antiseptic solely if necessary to prevent irritation.
- Apply a suitable dressing: Utilize a sterile bandage or non-adherent gauze to safeguard the laceration against bacterial contamination and promote a moist healing environment.
- Refrain from Picking or Scratching: Avoid the temptation to touch or remove scabs, as this may reopen incisions and elevate the likelihood of hypertrophic or keloid scarring.
Continuous Wound Care Management
- Hydrate and Moisturize: Apply topical ointments like petroleum jelly to help preserve moisture. Often, maintaining the wound in a hydrated state prevents crust formation and facilitates more rapid healing.
- Prevent Infection: Consistently monitor the lesion for signs of infection, such as redness, warmth, or abnormal discharge. Prompt treatment of infections can avert complications that may result in excessive scarring.
- Minimize Tension on Wounds: Refrain from vigorous activities that may strain the incision site, particularly in the case of surgical wounds. Mechanical stress on the epidermis may lead to the development of widened scars.
Lifestyle-Oriented Interventions
- Apply Sun Protection: Ultraviolet radiation exposure can intensify scars, rendering them more conspicuous. Apply a sunscreen with SPF 30 or higher to the affected, recuperating area.
- Maintain a Nutritious Diet: A well-balanced diet abundant in vitamins C, E, and zinc promotes your body’s collagen synthesis and facilitates tissue regeneration.
- Avoid Smoking: Smoking diminishes oxygen delivery to tissues and impairs wound healing, thereby elevating the risk of aberrant scarring.
Expert Interventions
- Massage Therapy: Gentle manipulation of the scarred area, as advised by a healthcare professional, can facilitate the gradual flattening of scars. Silicone sheets or gels: These products can help soften and diminish scars when applied consistently throughout the healing process.
- Consult a Plastic Surgeon Specialist: For high-risk lesions, seeking advice from a plastic surgeon can be beneficial to consider preventive interventions such as corticosteroid injections or laser therapy.
Implementing these measures during the initial phases of the wound-healing process can markedly diminish the complexity of scarring. Prevention requires vigilance and consistency to attain the most favorable outcome.
The Emotional and Psychological Effects of Scarring
Scars, whether enlarged, hypertrophic, or keloid, exert their effects well beyond the superficial layer of the skin. They may induce considerable emotional distress and psychological difficulties that differ based on an individual’s personal experiences, values, and the visibility of the scar. For numerous individuals, scars may function as unwelcome reminders of traumatic incidents, surgical procedures, or life-changing traumas, thereby hindering their capacity to progress.
Research has underscored the influence of societal beauty standards in influencing individuals’ perceptions of their scars. In societies or settings where smooth, blemish-free skin is highly valued, individuals may experience self-consciousness or diminished self-esteem. This is especially applicable to scars located in highly visible regions such as the face, neck, or palms. Feelings of humiliation, shame, or inadequacy frequently intensify in such situations, resulting in avoidance behaviors, social withdrawal, or challenges in establishing relationships.
The psychological effects of wounds extend beyond external perception; internal conflicts are equally significant. Scars can influence an individual’s sense of identity, particularly when they are linked to significant life experiences. Numerous individuals struggle with concerns regarding their body image, viewing their wounds as imperfections or blemishes. This internal struggle may give rise to anxiety, melancholy, or obsessive thoughts regarding the concealment of the scar.
Children and adolescents with scars encounter distinctive challenges, such as bullying and taunting by peers, which may exert lasting impacts on their emotional health. For adults, the process of acceptance frequently requires time and may necessitate emotional support or professional counseling. In severe instances, post-traumatic stress disorder (PTSD) may be associated with scars resulting from violent or traumatic events.
Addressing the emotional impact of wounds frequently requires a multidisciplinary approach. Dermatological treatments, psychological interventions, and peer support groups can all serve as valuable resources for individuals aiming to navigate the intricate emotional challenges associated with scarring.
Conclusion: Selecting the Appropriate Treatment Strategy
Choosing the most appropriate treatment strategy for widened, hypertrophic, or keloid scars requires a comprehensive approach that takes into account the scar type, individual skin features, and personal preferences. A comprehensive assessment conducted by a qualified plastic surgeon is vital to identify the most effective strategies for addressing the particular scar condition.
Widened scars, which frequently arise from tension during wound closure, typically respond effectively to minor revisions and non-invasive treatments. Options such as silicone sheeting, pressure dressings, or topical therapies may facilitate further improvement. In more severe instances, surgical procedures or dermal injections may be employed to aid in restoring the skin’s appearance.
Hypertrophic scars, distinguished by their elevated and erythematous appearance, generally respond to therapies focused on diminishing inflammation and collagen accumulation. Effective interventions may encompass corticosteroid injections, laser therapy, or cryotherapy. Pressure garments and silicone-based products may be advantageous for ongoing management and the prevention of recurrence.
Keloid scars, which frequently extend beyond the initial incision margins, often necessitate prolonged, multimodal treatment approaches. Initial treatment options may encompass corticosteroid injections, cryosurgery, or laser therapy. In resistant cases, surgical excision may be contemplated; however, surgery should be complemented with adjunctive treatments, such as radiation therapy or steroid administration, to prevent recurrence. Emerging therapies, such as 5-fluorouracil (5-FU) or interferon, offer supplementary options for complex cases.
When selecting a treatment, considerations such as the age and location of the scar, as well as the patient’s history of scarring, should inform the decision. Integrating multiple therapies may produce optimal results, while maintaining patience and realistic expectations can enhance the overall process. A customized approach is essential for effective scar management.

Figure #10: Picture of Dr. J. Timothy Katzen’s office in Beverly Hills. The address is 9735 Wilshire Boulevard, Suite #407, Beverly Hills, CA 90212. Phone is (310) 859-7770.
If you or someone you know has a widened, hypertrophic, or keloid scar, please get in touch with Dr. Katzen. Dr. Katzen and his team will be able to evaluate the scar and provide the most appropriate treatment. Please arrange for a consultation with Dr. Katzen by calling (310) 859-7770 or emailing [email protected]. Physical or virtual consultation can be arranged. Dr. Katzen is located in Beverly Hills, CA.