Understanding Post-Operative Pain: What to Expect After Plastic surgery
8/15/2025
Figure #1: Picture of a nerve sending pain messages. Created by DALL-E on 2/5/2025.
Post-operative pain is an expected part of the recovery process following plastic surgery. The degree of discomfort experienced depends on multiple factors, including the type of procedure performed, the patient’s pain tolerance (which is their ability to endure pain), and the overall complexity of the surgery. Recognizing what is normal and how pain evolves helps patients prepare for recovery.
Initially, the most intense discomfort is likely to occur within the first 48 to 72 hours following the procedure. This pain is often described as aching, throbbing, or tightness in the affected area, depending on the nature of the surgery. For example, procedures involving deeper tissue
manipulation, such as tummy tucks or breast augmentations, may result in a more pronounced sensation of pressure compared to surface-level procedures like dermabrasion.
During the first week post-surgery, swelling, bruising, and tenderness are typical. Pain may fluctuate during this time as surgical incisions begin to heal and internal tissues adjust. Over-the-counter or prescribed medications are commonly used to minimize discomfort. For more invasive procedures, plastic surgeons may prescribe stronger pain relievers to help control symptoms during the acute recovery phase.
By the second week, the intensity of the pain often diminishes significantly. Instead of sharp or throbbing sensations, patients may notice residual soreness or stiffness. Some procedures can lead to temporary nerve-related discomfort, such as tingling or numbness around the surgical area. These sensations generally subside with time.
While mild pain and sensitivity may linger for weeks or even months in more extensive surgeries, chronic or worsening pain should prompt immediate communication with your plastic surgeon. Identifying potential complications, such as infections or nerve damage, ensures timely intervention and improves long-term outcomes. Understanding the timeline for pain progression can alleviate anxiety and support a smoother recovery process.

Figure #2: The role of pain management. Created by DALL-E on 8/18/2025.
The Role of Pain Management in a Smooth Recovery
Effective pain management is crucial for ensuring a smooth recovery after plastic surgery. By addressing pain appropriately, patients can experience improved mobility, reduced risk of complications, and a more effective recovery. It’s important to remember that pain, if unmanaged, can interfere with the ability to rest, follow post-operative care instructions, and participate in light activities that promote healing. Following post-operative instructions is key to a successful recovery.
One of the primary benefits of comprehensive pain management is that it helps to minimize inflammation and discomfort during the critical healing period. Managing swelling and tenderness around surgical areas allows for better blood circulation, assisting in tissue repair and reducing the likelihood of infections.
Medication plays a significant role in controlling post-operative pain. Typically, plastic surgeons prescribe a combination of solutions tailored to individual needs. Six levels of pain medications are prescribed, including:

Figure #3: On-Q Pain pump can reduce post-operative pain by delivering local anesthetics for up to five days.
-
Local anesthetics: These may be administered during or after surgery to block pain signals temporarily in the affected area. These medications include lidocaine and marcaine. Post-operative lidocaine can be delivered can be delivered through a novel device called an ON-Q pain pump. Local anesthetic pumps can last up to five days.
Figure #4: Oral medication can alleviate post-op pain. Created by DALL-E on 8/18/2025.
-
Non-opioid analgesics: Medications like acetaminophen are commonly recommended for mild to moderate pain due to their anti-inflammatory properties.
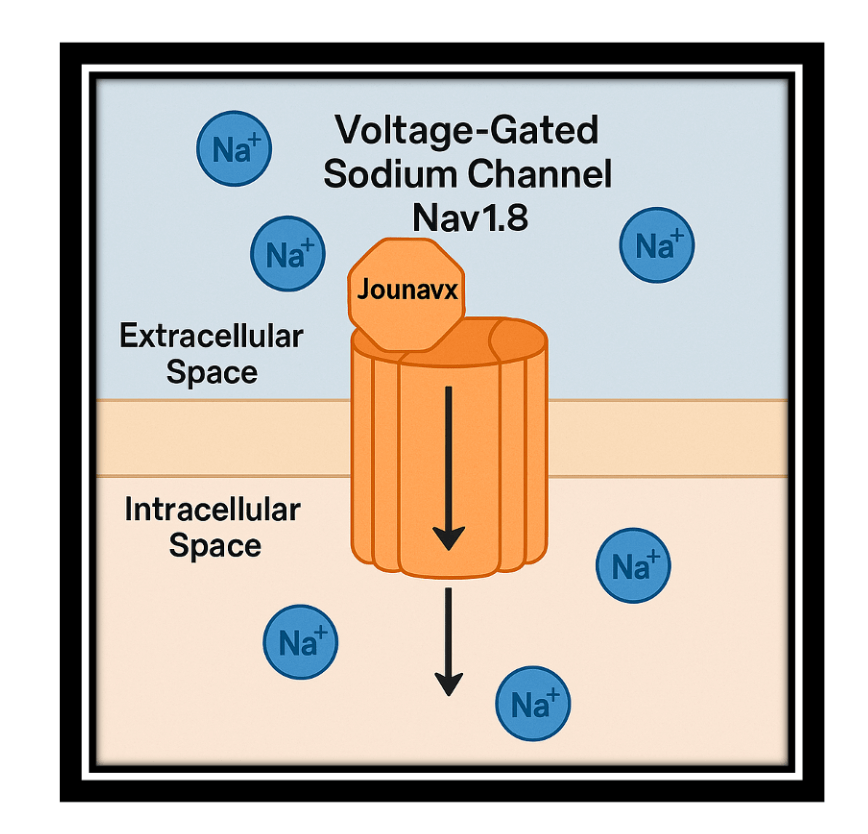
Figure #5: Journavx is the first peripheral nerve blockers. Journavx blocks pain messages from being sent to the brain by blocking peripheral sodium channels. Created by DALL-E on 8/18/2025.
-
New sodium channel blocker: Journavx is a new pain pill that blocks pain messages being sent to the brain. Journavx is an excellent addition to the treatment of post-operative pain. Journavx is a great non-opioid alternative for pain management.
-
Muscle relaxants: Plastic surgeons often prescribe muscle relaxants after a tummy tuck or lower body lift to help relax muscle tightness. Usually, muscle relaxants are used to treat pain associated with muscle tightness after plastic surgery procedures. A common muscle relaxant prescribed is Flexeril.
-
Oral opioid medications: In cases of more intense pain, short-term opioid use may be prescribed to provide relief while minimizing overuse risks. Medications in this class include Percocet (oxycodone and Tylenol) and Norco (hydrocodone and Tylenol).
-
Injection of opioid medication: In cases of severe pain, medications can be injected by a licensed nurse in an accredited facility. These medications include Demerol and Dilaudid.
Adherence to the prescribed medication regimen is critical. Irregular use of pain relief options can lead to unnecessary discomfort and hinder the body’s natural healing mechanisms.
Non-medical interventions also play a significant role in pain management. Techniques such as deep breathing exercises, meditation, and short, guided walking sessions can help alleviate pain perception. Staying hydrated and maintaining a nutritious diet support overall recovery efforts by strengthening the immune system and promoting tissue regeneration. These non-medical interventions can be used in conjunction with prescribed medications to enhance pain management and promote a smoother recovery.
By prioritizing effective pain control, patients are better equipped to focus on restorative care and the gradual improvement of their physical and emotional well-being post-surgery.
Types of Pain Associated with Plastic Surgery Procedures
Pain experienced after plastic surgery varies in intensity, location, and duration based on the type of procedure performed. Pain is also subjective. That means one person’s interpretation of pain is different from another person’s perception of pain. Understanding the types of pain associated with various surgeries can help patients prepare for the recovery process and manage discomfort effectively.

Figure #6: Incisional pain is one of six different types of post-operative pain. Created by DALL-E on 8/18/2025.
-
Incisional Pain: Incisional pain is the most common type of pain following plastic surgery. Incisional pain occurs at the site of the surgical incision and is characterized by sharp, localized discomfort. This pain is often due to the cutting of skin, underlying tissues, and sometimes muscle structures. This type of pain tends to subside as the incision heals, but may persist for a few weeks depending on the complexity and depth of the surgery.
-
Muscle Pain: Certain procedures, such as tummy tucks (abdominoplasty), lower body lifts, or breast augmentation involving the chest muscle, can lead to muscle pain. Patients often report soreness, tightness, or cramping in the affected area. This type of pain typically results from muscle manipulation, tension, or tightening during the surgical process.
-
Nerve Pain: Nerve pain, or neuropathic pain, may occur during or after the healing process due to nerve irritation or damage. This type of pain can manifest as burning, tingling, or shooting sensations. It’s important to note that procedures involving the face, such as rhinoplasty or facelifts, are more likely to result in temporary nerve-related discomfort as the nerves regenerate. This discomfort is a normal part of the healing process and usually subsides over time.
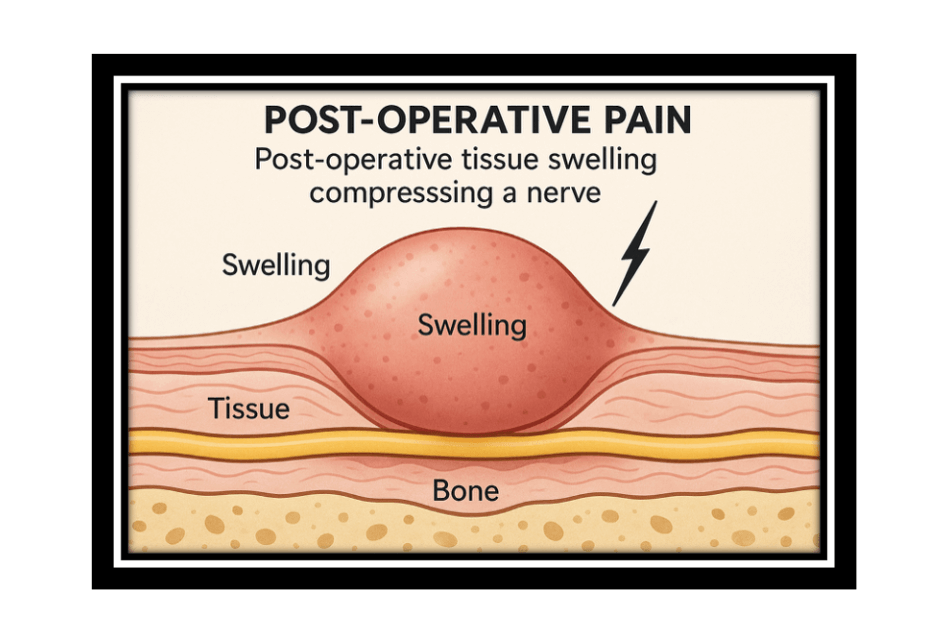
Figure #7: Swelling or post-operative edema can press on surrounding tissues including nerves.
Sometimes, these compressed nerves can signal localized pain. Created by DALL-E on 8/18/2025.
-
Swelling-Related Pain: Swelling in the recovery phase often causes discomfort or a dull, throbbing pain. This type of post-operative pain is a common response to inflammation following procedures such as liposuction, breast surgery, or facelifts. Effective use of compression garments, foam, lymphatic massage, and prescribed medications can help alleviate this type of pain.
-
Pressure or Heaviness: Patients undergoing procedures like breast reconstruction or augmentation may report a sensation of pressure or heaviness. This is often due to the placement of implants or adjustments made to the body’s normal structure. Such pain typically improves as the body adjusts to these changes over time.
-
Generalized Discomfort: Fatigue and mild, widespread discomfort are common after major surgeries like body contouring and are frequently linked to the body’s inflammatory response. This pain can affect areas separate from the surgical site due to compensatory movements, which are the body’s natural adjustments to protect the surgical area, or prolonged immobility during the healing period. Understanding these sources of pain can help patients adjust their post-operative activities to minimize discomfort and promote a smoother recovery.
Understanding these differing types of pain can aid in tailored pain management strategies for improved recovery outcomes.
Preparing for Pain Management Before Plastic Surgery
Proper preparation for pain management before plastic surgery is a critical step in ensuring a smoother recovery process. Patients should discuss their concerns and expectations about post-operative pain with their chosen plastic surgeon during pre-surgical consultations. This is the ideal time to establish a pain control plan tailored to the individual’s needs, health history, and the specific procedure being performed.

Figure #8: Pre-operative planning is essential to anticipate and control post-operative pain.
Photo by Alexandr Podvalny on Unsplash.
-
Pre-Surgery Evaluation and Planning: Patients must undergo medical assessments to identify any underlying conditions that could affect pain tolerance or medication efficacy. Factors such as allergies to certain medications, prior reactions to anesthesia, and pre-existing pain disorders should be disclosed to the surgical team. Open communication between the patient and the healthcare provider allows for a personalized approach to pain relief, incorporating both pharmacological and non-pharmacological methods when necessary.
-
Medication Pre-Planning: Plastic surgeons often prescribe pain medications before surgery to prepare for post-operative pain management. These may include anti-inflammatory drugs or painkillers, which are meant to minimize discomfort in the initial recovery phase. Patients should receive detailed instructions on how to use these medications, including timing, dosages, and potential interactions and side effects. In certain cases, preemptive dosing strategies may be implemented to reduce the intensity of pain immediately after surgery.

Figure #9: Patient should discontinue alcohol and smoking before plastic surgery. Created by DALL-E on 8/18/2025.
-
Lifestyle Adjustments: Lifestyle preparations before surgery can also greatly influence the effectiveness of pain management. Avoiding alcohol and tobacco is recommended, as these substances can interfere with healing and amplify pain. Incorporating light physical activity or relaxation techniques, such as deep breathing exercises, may help improve overall pain resilience following the procedure.
-
Addressing Psychological Factors: Stress and anxiety can worsen the perception of pain. Before surgery, patients may benefit from engaging in techniques to promote mental well-being. Activities such as guided meditation, visualization, or even professional counseling sessions can help manage pre-operative stress, potentially improving the recovery experience.
Underpinning the preparation process is the need for patients to fully understand the importance of adhering to their plastic surgeon’s instructions and following the established pain management plan.
Medications Commonly Used for Post-Operative Pain Control
Figure #10: Medications needed for post-operative pain control. Created by DALL-E on 8/18/2025.
Effective post-operative pain management is critical for recovery following plastic surgery. A variety of medications, tailored to the patient’s needs and the type of procedure, are commonly used to alleviate discomfort during the healing process. These medications target varying levels of pain and work through different mechanisms of action.
-
Opioids: Opioids are often prescribed for acute post-operative pain. These are potent medications that block pain signals in the brain and spinal cord. However, their usage is typically limited to short durations due to potential side effects, including drowsiness, constipation, nausea, or the risk of dependency.
-
Acetaminophen (Tylenol): Acetaminophen is a generally safe and well-tolerated option for managing mild pain. It is often used in conjunction with other medications, such as opioids, to enhance pain relief. Acetaminophen does not reduce inflammation but offers significant benefits for managing general soreness without the risk of blood thinning.
-
Muscle Relaxants: Often during plastic surgery procedures, like tummy tucks and body lifts, muscles are tightened. Also, in a reaction to localized pain, some patients constrict surrounding local muscle as a local reaction and in an attempt to decrease pain. To relieve pain associated with muscle tightening whether mechanical or induced, some plastic surgeons prescribe muscle relaxants like Flexeril.
-
Local Anesthetics: Local anesthetics, like bupivacaine or lidocaine, are frequently administered during surgery or immediately afterward. After surgery, the ON-Q pump can effectively deliver local anesthetics for many days after the procedure. The ON-Q pain pump can be used for procedures like a tummy tuck, body lift, back lift, thigh lift, or even breast procedures. These medications provide targeted pain relief at the surgical site and are especially helpful for controlling pain in the early recovery period. Extended-release formulations (like Marcaine and Exparel) may be used to improve their duration of action. However, the ON-Q pain pump usually lasts longer than the extended-release local anesthetics.
-
Nerve Pain Medications: For surgeries associated with nerve pain, medications such as gabapentin or pregabalin may be included. These drugs minimize nerve irritation by regulating pain signals. They are particularly effective for managing neuropathic pain following procedures involving tension on nerves or intricate reconstruction.
Careful consideration of the type, dosage, and combination of these medications ensures patients experience minimal discomfort and a smoother recovery process.
These pain medications will be used in the treatment of post-operative pain. These medication will be used at the appropriate time to treat the type of post-operative being experienced. A patient should learn to recognize the type of pain they have and medicate appropriately.
Progression of Pain and Timing of Pain Medication
During your healing after a plastic surgery procedure, you will experience pain. For some, the pain will be minimal; for others the pain will be more severe. Patients should learn to identify increasing pain and be prepared to treat accordingly.
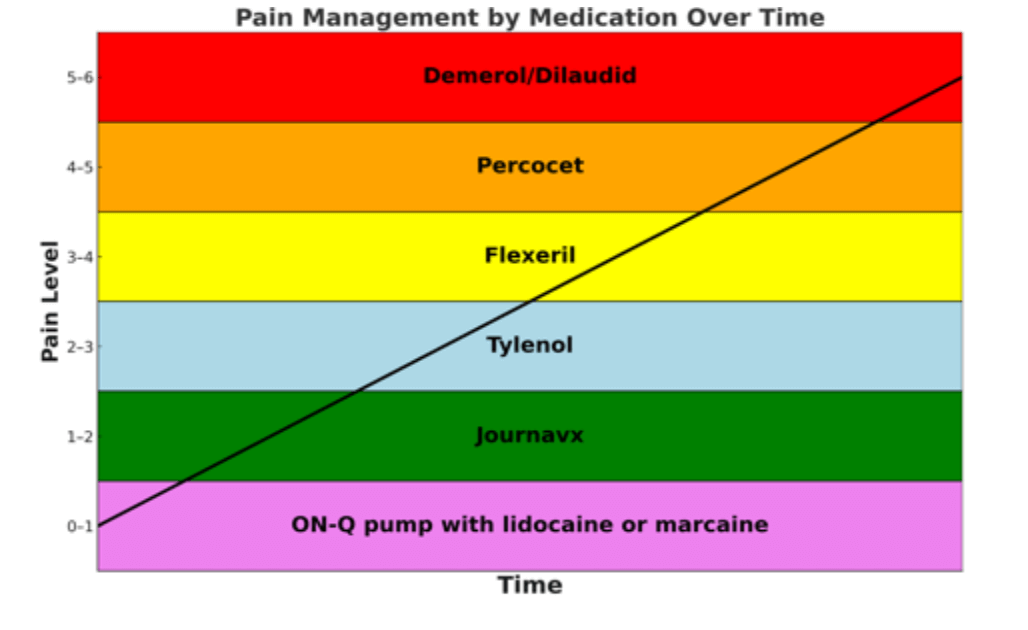
Figure #11: Depiction of the progression of pain and medications to treat the appropriate severity of pain. Created by DALL-E on 8/19/2025.
After your surgery, much of the pain with be managed with the ON-Q pain pump and scheduled intake of Journavx. As time progresses and the pain increases, you will need stronger medications. Usually, patients progress to Tylenol and a muscle relaxant, like Flexeril. If the pain becomes extreme, you may require occasional opioids like Percocet, Demerol, or Dilaudid.
Non-Medical Pain Relief Techniques: Complementary Approaches
Non-medical pain relief techniques serve as complementary methods to manage discomfort after plastic surgery. These approaches can help reduce pain perception, promote relaxation, and support the healing process when used alongside prescribed medical treatments. While they are not substitutes for professional medical advice, they can provide significant relief to patients seeking holistic ways to improve their post-operative experience.
-
Meditation and Deep Breathing Exercises: Techniques such as mindfulness meditation and diaphragmatic breathing can lower stress, reduce muscle tension, and diminish the intensity of pain perception. Guided meditation sessions, specifically designed for post-surgical pain relief, can teach patients techniques to stay calm and focused during recovery. Deep breathing also helps calm the nervous system and promotes better oxygenation of tissues, which may aid in tissue repair.
-
Aromatherapy: Using essential oils, such as lavender or chamomile, may complement pain management through relaxation. When used in a diffuser or combined with massage oils, aromatic compounds can reduce stress and provide calming effects on the body and mind. While aromatherapy is typically safe, patients should ensure they are not allergic to specific scents before using them.

Figure #12: Massage therapy can decrease pain. Created by Midjourney 5/13/2025
-
Massage Therapy: Pending approval from your plastic surgeon, a gentle massage near—but not directly on—the surgical site may improve circulation and ease muscle tension. This technique can promote lymphatic drainage, reducing fluid retention and swelling. Special post-surgical therapeutic massages, such as lymphatic drainage massage, may offer targeted relief under professional supervision.
-
Music Therapy: Listening to soothing music has been shown to lower cortisol levels and decrease pain-related stress. Curated playlists of calming or soft instrumental music can enhance the patient’s overall comfort during recovery. Music therapy can be used both during moments of rest and in tandem with meditation or other relaxation practices.
-
Acupressure: Acupressure targets specific energy points in the body to provide relief. Using gentle pressure on prescribed points may help decrease pain and inflammation for some patients. Practitioners commonly recommend it as a safe alternative for those looking to control discomfort without additional medications.
-
Over-the-Counter Topical Remedies: Natural topical products, such as arnica gel or creams containing menthol, can provide localized relief when applied around—never directly on—the surgical site. These formulations may ease soreness and reduce bruising while adhering to healing protocols prescribed by the healthcare provider.
-
Hyperbaric therapy: Healing can be accelerated by delivering oxygen to your healing tissues. One method to increase tissue oxygenation is by increasing the surrounding air pressure to force oxygen into your tissue. Increased air pressure is accomplished in a dedicated steel hyperbaric chamber. Typical hyperbaric treatments last 60 to 90 minutes.
Integrating these non-medical techniques into a post-operative regimen may offer patients greater control over their comfort levels, allowing them to focus on recovery milestones.
The Importance of Rest and Recovery for Pain Reduction

Figure #13: Rest is an important part of your post-operative healing and pain control. Created by DALL-E on 8/19/2025.
Rest and recovery are integral components of the healing process following plastic surgery. The body requires adequate time to repair tissues, reduce inflammation, and restore its strength. Insufficient rest can hinder these processes, potentially delaying recovery and prolonging post-operative pain.
Physical rest allows surgical wounds and the surrounding tissues to repair themselves effectively. Tissue damage caused during surgery triggers the body’s natural healing mechanisms, including the production of collagen and the remodeling of tissue. Overexertion during the initial healing period can disrupt these processes, exacerbate swelling, and elevate discomfort levels.
Equally critical is mental and emotional rest, which directly influences the body’s ability to recover. Stress and anxiety can increase muscle tension, raise cortisol levels, and heighten the perception of pain. Creating a calm and relaxing environment promotes mental well-being and helps reduce pain sensitivity during recovery.
Physicians often recommend that patients follow specific guidelines to optimize the benefits of rest. These may include:
-
Maintaining a sleep schedule: Sleep is when the body focuses most intensively on cellular repair and inflammation reduction.
-
Avoiding strenuous activities: Activities such as heavy lifting, bending, unnecessary exercise or excessive movement can strain the surgical site and amplify pain.
-
Elevating the body as advised: For procedures involving the face, abdomen, or other specific areas, elevating certain body parts can help minimize post-operative swelling and discomfort.
Patients are also advised to heed their body’s signals. Signs such as fatigue or increased pain indicate a need for more rest. Over time, as the healing progresses, light movements or doctor-recommended exercises can be gradually introduced.
Rest is not a passive step in recovery but a proactive measure to minimize pain and promote efficient healing. Proper rest and recovery practices not only reduce discomfort but also minimize complications, contributing to better overall outcomes.
Recognizing Signs of Complications Related to Pain
Figure #14: Monitoring your pain level is an important part of healing process. Photo by National Cancer Institute on Unsplash.
Post-operative pain is a normal part of the healing process, but certain signs may indicate complications requiring immediate medical attention. Patients, caregivers, and medical professionals must be vigilant in identifying symptoms that fall outside the expected range of post-surgical pain.
Early Warning Signs to Monitor
-
Sudden Increase in Pain: Pain intensity should gradually decrease over days or weeks following surgery. A sharp or unexpected increase in pain levels may suggest complications such as infection, hematoma, or nerve injury.
-
Redness and Swelling: While some redness and swelling are expected, excessive or spreading redness, accompanied by warmth or extreme tenderness, could be indicative of an infection or inflammatory response.

Figure #15: If you have a fever of 101°F (38.3°C), call your plastic surgeon. Created by DALL-E on 8/18/2025.
-
Fever: A post-operative fever beyond 101°F (38.3°C), especially when combined with increased pain, may signal infection, even if the surgical site appears normal.
-
Drainage and Odor: Foul-smelling discharge or pus from the incision site often points to wound infections. Clear or slightly yellow fluid may be harmless, but it should still be discussed with a healthcare provider.
-
Unrelieved Pain Despite Medication: If prescribed pain relief measures fail to provide comfort, this could suggest underlying issues such as improperly managed nerve pain, compartment syndrome, or other surgical complications.
Symptoms of Specific Complications
-
Nerve Damage: Tingling, numbness, or sharp, shooting pains that persist or worsen over time can indicate nerve injury or neuropathic pain.
-
Deep Vein Thrombosis (DVT): Localized pain, warmth, and swelling in the leg, particularly after plastic surgery on the lower body, may be signs of a blood clot and warrant emergency evaluation.
-
Tissue Necrosis: Dark discoloration, unusual firmness around the surgical site, or malodorous symptoms may suggest inadequate blood flow to tissues, leading to cell death.
Seeking Immediate Medical Attention
Persistent symptoms or the combination of several concerning signs should never be ignored. Patients should contact their surgical team or an emergency department if they experience severe pain coupled with symptoms such as difficulty breathing, fainting, or swelling that rapidly worsens. Evaluating and addressing complications promptly can prevent long-term damage and improve overall recovery outcomes.
Tips for Communicating Effectively With Your Plastic Surgeon About Pain Levels
Effective communication with a plastic surgeon about post-operative pain is essential to ensuring proper pain management and recovery after plastic surgery. Patients can take the following steps to ensure their concerns are heard and appropriately addressed:
-
Prepare Specific Details: Before the appointment, patients should note the location, intensity, frequency, and triggers of their pain. Using descriptive terms like
“sharp,” “burning,” or “throbbing” provides more clarity. Keeping a pain diary can help document patterns or changes.
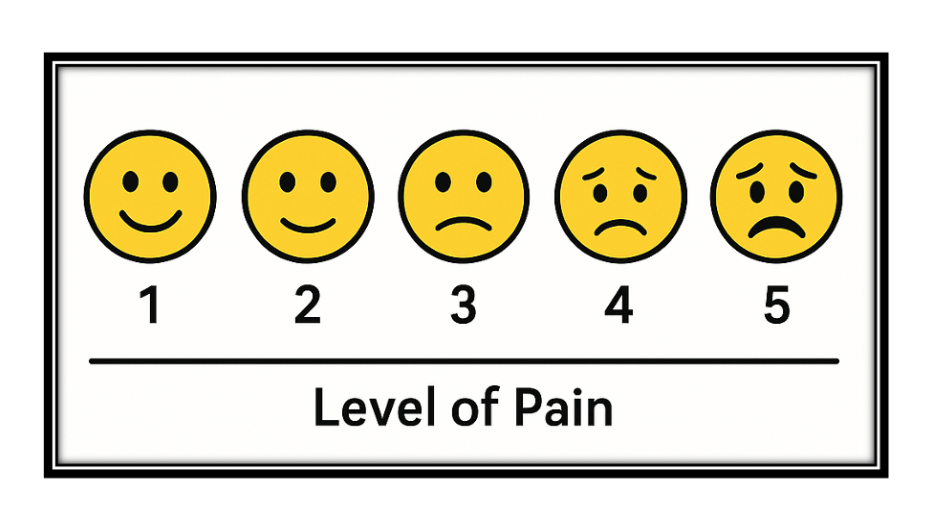
Figure #16: The importance of standardizing pain with a smiling face scale. Created by DALL-E on 8/18/2025.
-
Use Visual Aids or Pain Scales: Referring to a standardized pain scale, such as a 0–5 numeric rating or a simple facial expression chart, can help quantify pain. This helps plastic surgeons better understand and compare pain levels objectively.
-
Avoid Downplaying Symptoms: It is critical to be honest about pain levels, even if the discomfort seems minor or tolerable. Downplaying symptoms may result in inadequate pain management or delayed identification of complications.
-
Ask Questions About Medications and Alternatives: Patients should inquire about prescribed pain medications, potential side effects, and non-pharmaceutical options like ice therapy, elevation, or relaxation techniques.
-
Discuss Expectations and Concerns: Openly discussing expected healing timelines, concerns about side effects, or fears surrounding pain management fosters trust and creates a more collaborative approach.
-
Stay Calm and Professional: Maintaining a respectful tone, even when frustrated, facilitates a more productive dialogue. Plastic surgeons are more likely to engage constructively when patients communicate clearly and calmly.
-
Follow Up as Necessary: If pain persists or worsens, updating the plastic surgeon promptly ensures timely intervention. Patients should systematically provide updates to help their plastic surgeon assess whether the recovery process is on track.
These strategies optimize the relationship between patients and plastic surgeons, enabling tailored care and more effective pain management.
Long-Term Pain Management: What to Expect Weeks After Plastic Surgery
In the weeks following plastic surgery, pain management enters a new phase. While many patients experience significant improvement in discomfort during this period, it is common for residual soreness, stiffness, or sensitivity to persist. Understanding how to navigate these symptoms is essential for a smooth recovery process.
Pain that lingers beyond the initial acute phase is often associated with tissue healing. As nerves regenerate and scar tissue forms, tingling, pulling sensations, or mild shooting pains may occur. Patients are often advised to use over-the-counter medications to alleviate minor discomfort. For some, doctors may provide prescriptions for mild muscle relaxants if spasms contribute to pain. Swelling at the surgical site may persist for weeks, contributing to pressure or tightness. Elevating the area (if applicable), wearing compression garments as directed, and engaging in light, approved physical activity can help manage these sensations. Massage techniques or lymphatic drainage, when cleared by a medical professional, may also aid in reducing swelling and associated pain.
Patients may experience emotional or mental fatigue due to prolonged discomfort. Stress-reduction strategies, such as mindfulness techniques, breathing exercises, or counseling, can help minimize the psychological effects of chronic pain. Some individuals may find complementary therapies, such as acupuncture, beneficial during this stage, though these should only be pursued under medical recommendation.
Follow-up appointments remain critical during this period. Persistent severe pain, signs of infection, or unusual sensations may indicate complications requiring prompt medical intervention. Communication with the surgical team ensures that pain and healing are appropriately monitored.

Figure #17: Dr. Katzen’s Beverly Hills office at 9735 Wilshire Boulevard, Suite 407, Beverly Hills, CA 90212
If you have any other questions about post-operative plastic surgery pain control or plastic surgery in general, please contact Dr. J. Timothy Katzen at (310) 859-7770. If you or someone you know is considering plastic surgery, please get in touch with Dr. J. Timothy Katzen or email scheduling@timothykatzenmd. Dr. Katzen can meet with you in his office located in Beverly Hills. Alternatively, Dr. Katzen can arrange a virtual consultation on Zoom, FaceTime, and WhatsApp.